Short Trunk Dwarfism and Kyphoscoliosis are the First Alarming Signs in Children with Kozlowski Type of Spondylometaphyseal Dysplasia
Abstract
Background: In early childhood
moderate short trunk dwarfism associated with spine misalignment can occur in a
number of heritable bone disorders. Later on, scoliosis or kyphoscoliosis
associated with curved limbs associated with waddling gait evolved. Stubby
hands and feet with stiff joint movements associated with gait disturbance are
additional abnormalities which manifest itself during the course of the
disease. Clinical and radiological phenotypic characterizations are the
baseline tools to delineate and diagnose the different types of skeletal
dysplasia.
Patient and Methods: Short trunk dwarfism, progressive kyphoscoliosis
in a group of children with pre and postnatal growth retardation (two boys and
two girls and one adult unrelated parents (aged 6 -13 and a-33-year-old woman
have been enrolled in this study). Family history and radiographic
documentation revealed two parents of the two unrelated children are
manifesting typical phenotype akin to their children. Progressive kyphoscoliosis
deformity in a-6-year-old-boy (kyphosis 30°Cobb´s angle and scoliosis 20° and a 13-year-old girl kyphosis
- 70◦ Cobb’s angle and
scoliosis - 55◦ Cobb´s angle) were the
main deformity. Clinical and radiological phenotypic characterizations
were the baseline tool for management.
Results: The distinctive
clinical features in these children and adults were severe short trunk
dwarfism, prominent forehead/ frontal bossing, hyper lordosis and forearm
deformity. Waddling gait, restricted joint mobility and progressive
kyphoscoliosis were evident. Radiological phenotype revealed flattening of the
vertebrae with rounding of the anterior ends and posterior wedging. The pelvis
showed squared iliac wings, narrow sciatic notches, flat trident acetabular
roofs, short femoral necks resulted in coxa vara. The overall clinical and
radiological phenotype were compatible with the diagnosis of
Spondylometaphyseal dysplasia –Kozlowski type (SMD). Correction of kyphoscoliosis deformity has been successfully performed
in the 13-year-old-girl - «growing rod» construction. After 5 years the patient
performed staged operations. Final correction kyphoscoliosis deformity - final
posterior fusion Th2-L5 (posterior spondilodesis)
Conclusion: Three major skeletal problems have been seriously correlated to the SMD
Kozlowski type in our group of children and adults. Firstly, the early onset
progressive kyphoscoliosis, secondly odontoid hypoplasia with subsequent
development of os odontoideum with subsequent development of atlantoaxial
instability. Thirdly, the development of coxa vara which is correlated to
progressive rarefaction of the bone matrix. Furthermore, the lack of the normal
cohesiveness of the femoral necks in connection with metaphyseal dysplasia play
a negative role in the biomechanics of the locomotor system. In this study we
discussed the management of the musculoskeletal abnormalities in patients with
SMD Kozlowski type.
Keywords: Spondylometaphyseal, Dysplasia, Childhood, Adulthood
1. Introduction
Spondylometaphyseal dysplasia, Kozlowski type (SMD-Kozlowski) (OMIM 184252) is
characterized by a constellation of abnormalities noted in early childhood such
as moderate dwarfism, most marked in trunk region, short neck,
scoliosis/kyphoscoliosis, mildly curved limbs, short and stubby hands and feet.
The earliest sign of the disease is often growth retardation with spinal
kyphosis appearing around the age of 18 -24 months of age. Though several
reports showed that scoliosis of progressive nature was noted at birth1-3. Musculoskeletal
features of limitations in joint mobility associated with gait disturbance and
in some patient’s genu valgum. Progressive kyphoscoliosis, either manifested in
early childhood or late in adulthood4. The radiological phenotype is characterized by
generalized severe platyspondyly with increased height of the intervertebral
disc space, open staircase vertebral bodies, medially placed pedicles, scoliosis/kyphoscoliosis
and early osteoarthritic spine changes are common manifestations of the disease.
Broad
short basilar portion of the iliac bones, with broad horizontal acetabular
bones and horizontal acetabular roofs (these are mostly noted in children).
Progressive metaphyseal widening, sclerosis and irregularity causing
effectively the development of coxa vara. Coxa vara is a common finding which
is correlated to the irregular metaphyseal ossification in the tubular bones
(of maximal intensity in the proximal femora). The metaphyses are characterized
by widening, sclerosis and irregularity which effectively leads to the
development of coxa vara.)5-8. Congenital coxa vara
is commonly associated with a significant number of diverse forms of skeletal
dysplasia and in some can lead to limb-length discrepancy. An association
between coxa vara and abnormalities of development of the femur such as
congenital short femur, congenital bowed femur and proximal focal femoral
deficiency has long been recognised1-8. The autosomal dominant TRPV4
disorders are a group of skeletal dysplasia’s encompassing spondylometaphyseal
dysplasia Kozlowski type, spondyloepiphyseal dysplasia Maroteaux type,
Metatropic dysplasia and other disorders of neuromuscular origin. All these
disorders are caused by mutation in TRPV4 gene (OMIM 605427). Differentiation and diagnosis can only made
via clinical and radiographic phenotypic characterizations1-3, 9-11.
2. Patients and Methods
The study protocol was approved by Ethics Committee of the National Medical Research Center for Traumatology and Orthopedics, (number 4(50) issued on 13.12.2016) Kurgan, Russia. Informed consents were obtained from the patient’s Guardians to publish. Six patients (girls and 4 boys with age average of 3 years). We fully documented these children through detailed clinical and radiological phenotypic characterizations at the axial skeleton and neurosurgery department, Ilizarov Center, Russia. At birth babies showed pre and postnatal growth deficiency and later on in infancy children with SMD type Kozlowski syndrome manifested short trunk dwarfism. The clinical phenotype of the backbone in a-6-year-old-boy who showed short trunk dwarfism with no associated rhizomelia. Similarly, a-13-year-old –girl showed apparent trunk dwarfism associated with progressive kyphosis, though with normal length of the limbs (Figure 1a and b). Their subsequent course of development has been described as being retarded in acquiring motor skills. Spinal kyphosis/kyphoscoliosis appeared around the age of 18 to 24 months which is characterized as being of progressive nature. All our patients were products of uncomplicated gestation. All born full term, at birth the length and weight were around the 10th Percentile and OFC around the 25th percentile. Walking has been achieved around the ages of 15 to 18 months albeit with difficulties. Gait abnormalities predominate the motor activity followed later on by the development of progressive limp. At time of presentation all manifested proximal varus deformity with an angle of 80°. Limb length inequality was around the average of 2.5 cm to 3 cm. No particular cranio-facial dysmorphic has been noted. Musculoskeletal examination showed a positive Trendelenburg sign, abduction limited to 30° and internal rotation limited to 10° were present mostly on the left side. The right hip could be abducted 60° and internally rotated 35°. No ligamentous hyperlaxity but apparent joint stiffness has been noted. Upper limbs showed no abnormalities (except for stubby hands and feet). Neurological examination was normal. Hearing, vision and intelligence were normal. Examination of hair, teeth, nails and skin were normal. Laboratory studies showed normal white and red blood cell and platelet counts, normal serum calcium, phosphorus and alkaline phosphatase levels. Screening of urine for amino acids and mucopolysaccharides were negative and all manifested normal karyotype. Fluorescence In Situ Hybridization (FISH) tests showed normal results.
(a) (b)
Figure 1a): A-6-year-old-boy showed short trunk dwarfism with no associated rhizomelia. b): A-13-year-old –girl showed marked short trunk dwarfism associated with progressive kyphosis with normal limb lengths.
3. Results
In accordance with the aforementioned clinical features, the radiological phenotype has been performed to further interpret the constellation of the skeletal abnormalities. Lateral thoracic spine radiograph of a-six-year-old-boy with SMD (Kozlowski type) showed generalized platyspondyly (flat vertebral bodies) (a). AP hand radiograph of a-12-year-old-boy with SMD (Kozlowski type) showed small carpal bones, retardation of the carpal ossification’s centres with minimal metaphyseal changes of the short tubular bones which look short and broad. Note marked metaphyseal dysplasia of the inferior ends of the radius and ulna (Figure 2a and b). Lateral spine radiograph of a -13-year-old-girl with the diagnosis of SMD type Kozlowski showed evident generalized platyspondyly with anterior wedging (a). Note, severe kyphoscoliosis deformity. (kyphosis - 70◦ Cobb and scoliosis - 55◦ Cobb) (Preoperative radiographs) (Figure 3a and b). Postoperative spine radiographs showed correction kyphoscoliotic deformity - «growing rod» construction. For 5 years the patient performed staged operations. final correction kyphoscoliotic deformity - final posterior fusion Th2-L5. Posterior spondilodesis (Figure 4a and b).
(a) (b)
Figure 2: a) Lateral thoracic spine radiograph of a-six-year-old-boy with SMD (Kozlowski type) showed generalized platyspondyly (flat vertebral bodies). b) AP hand radiograph of a-12-year-old-boy with SMD (Kozlowski type) showed small carpal bones, retardation of the carpal ossification’s centres with minimal metaphyseal changes of the short tubular bones which look short and broad. Note marked metaphyseal dysplasia of the inferior ends of the radius and ulna.
(a) (b)
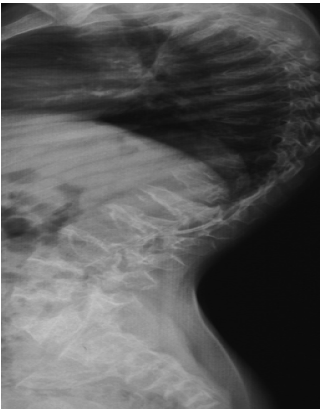
Figure 3: a) Lateral spine radiograph of a -13-year-old-girl with the diagnosis of SMD type Kozlowski showed evident generalized platyspondyly with anterior wedging. b) Note, severe kyphoscoliosis deformity. (kyphosis - 70◦ Cobb and scoliosis - 55◦ Cobb)( Preoperative radiographs).
(a) (b)
Figure 4: a) Postoperative spine radiographs showed correction kyphoscoliotic deformity - «growing rod» construction. b) For 5 years the patient performed staged operations. final correction kyphoscoliotic deformity - posterior fusion Th2-L5. Posterior spondilodesis.
4. Discussion
Spondylometaphyseal
dysplasia is a heterogeneous group of disorders characterised by platyspondyly
and metaphyseal changes not unlike those of Schmid’s metaphyseal
chondrodysplasia12. Spondylometaphyseal dysplasia has been discussed by various authors by
whose names are well known such as Kozlowski1, Sutcliffe13, Murdoch and Walker14, Borochowitz15, Wiedemann and
Spranger16. Kozlowski type of
spondylometaphyseal dysplasia can manifest itself early on in life or later in
life. Spondylometaphyseal dysplasia Kozlowski type has been published by
various authors. A series of further cases was described by Krakow et al.17. Four of patients had
typical findings that included scoliosis, a waddling gait and radiologically,
platyspondyly, over faced vertebral pedicles, flared iliac wings, a mildly
flattened acetabular roof and irregular capital femoral metaphysis and delayed
carpal ossification. Some had findings akin to non-lethal metatropic dysplasia.
Heterozygous mutations in TRPV4 (as in metatropic dysplasia and mild autosomal
dominant brachyolmia) were found in some patients. The differential
diagnosis of patients with SMD-Kozlowski type has to be made with metatropic
dysplasia (which differs by the presence of dumb-shaped long tubular bones and
more severe epiphyseal dysplasia as well as crescent shaped iliac wings18,19. Kozlowski type SMD
should also be differentiated from Spondylo-chondrodysplasia20.
Dyggve-Melchior-Clausen syndrome (Smith-McCart dysplasia), which does not
include mental retardation, should be included in the differential diagnosis21. Spondylometaphyseal
dysplasia cone –rod dystrophy is another entity akin to SMD Kozlowski type c
but in the former lateral views of the spine showed ovoid shaped vertebral
bodies rather than flat as seen in the latter22.
Spondyloepimetaphyseal dysplasia type Maroteaux shows varying degrees of
platyspondyly with less metaphyseal and more epiphyseal involvement23.
Kyphosis presenting at birth or before adolescence is
almost always due to congenital anomaly of vertebral development. The causation
and pathogenesis of congenital kyphosis/ scoliosis and or kyphoscoliosis are
arise from either a dysplastic process or from vertebral malsegmentation.
Scoliosis and kyphoscoliosis are a symptom complex in more than 742 syndromic
entity24.
Coxa vara is defined as a decrease in the angle between the head or neck and shaft of the femur, often in presence of a metaphyseal defect. In other words, the neck-shaft angle is less than 110°. It is characterised by a decrease in the neck-shaft angle and clinically by a waddling gait or limb length discrepancy. Symptoms do not develop until the child starts to walk and often not before the age of 3 or 4 years. Coxa vara is a constant finding in many types of skeletal dysplasia as part of the manifestations of a generalized growth disturbance. Symptoms of coxa vara do not develop until the child starts to walk and often not before the age of 3-4years. There is a typical limp or a waddling gait resembling that of dysplastic developmental dislocation of the hip. Abduction of the hip is limited; there is a positive Trendelenburg's sign on standing on the affected side and the greater trochanter is elevated. It has been suggested that abnormal development of the proximal femoral cartilaginous physis and defective ossification of the adjacent metaphysis are responsible for the progressive decrease of the neck shaft angle25,26. Oh, et al.27 studied 46 patients with coxa vara. Spondyloepiphyseal dysplasia congenita or spondyloepimetaphyseal dysplasias were the forms of osteochondrodysplasias reported in connection with congenita coxa vara. They concluded that the lack of the epiphyseal ossification was the most challenging element. Further studies indicated that histological investigations revealed abnormalities in the proximal femoral physeal chondrocyte maturation, with disruption of the normal columnar architecture and abnormal calcification of the cartilaginous matrix. This abnormal endochondral ossification resulted in decreased production of the metaphyseal bone, leading to relative osteoporosis and subsequent weakness in this area. Patients with coxa vara and a Hilgenreiner angle greater than 60 degrees are candidates for a surgical intervention, as are patients with a Hilgenreiner angle greater than 45 degrees who are symptomatic presenting with limping or showing progression. Surgical correction is performed by a valgus osteotomy according to Pauwels (VY osteotomy with plate fixation). Malalignment of the leg can be treated by gradual correction using 8-plates, as long as the epiphseal growth plates are open. The surgical correction of limb length inequality by lengthening procedures is risky. Prerequisite for indication should be absolute stability of hip and knee joints28,29.
Congenital kyphosis/kyphoscoliosis and Coxa vara are almost always a symptom complex rather than a separate diagnostic entity until proven otherwise. Kyphosis present at birth or in pre-adolescence is almost always due to a congenital anomaly in correlation with vertebral mal-development (genetically programmed). The deformity may be purely kyphotic or, more commonly, combines kyphosis and scoliosis. The vertebral bodies mal-development in patients with skeletal dysplasia is part of the entire growth disturbance of the skeletal system, which is totally different from other forms of vertebral abnormalities as seen in dozens of syndromic entities in which vertebral dyssygmentations (failure of segmentation) as in block vertebrae is part of the symptom complex in. Coxa vara can be clinically classified as developmental, congenital, dysplastic or traumatic and may occur at the physis or in the trochanteric or subtrochanteric area. Skeletal dysplasia, in particular, can manifest a wide range of variable and confusing phenotypic features, varying from profound dwarfism, lethal in utero, to phenotypically normal individuals but with a genetically programmed disorder of unpredictable onset and form. Clinico-radiographic documentation is the base line for proper management. Our paper might indicate an area of concern to generate further research that it could lead to elaborate knowledge.
6. References
- Kozlowski K,
Maroteaux P, Spranger JW. La dysostose spondylometaphisaire. Presse Med. 1967;75: 2769.
- Guzman CM, Aaron GR. Spondylo-metaphyseal dysplasia
(Kozlowski type): case report. Pediatr Dent. 1993;15: 49-52.
- Verloes A, Lepage P, Baumann C, et al.
Spondylometaphyseal dysplasia, East-African type: a new form of early, severe
SMD with rounded vertebrae. Am J Med Genet. 2002; 113:362-366.
- Lachman R. The spondylometaphyseal
dysplasia’s. Clinical, radiological and pathologic correlation. Ann Radiol
(Paris). 1979;22: 125-135.
- Lequesne GW, Kozlowski K. Spondylometaphyseal dysplasia. Br J Radiol.
1973;46:685-691.
- Kozlowski K, Beemer FA, Bens G, et al. Spondylometaphyseal dysplasia (report of 7 cases and
essay of classification). In: Papadatos CJ, Bartsocas CS (eds). Skeletal
Dysplasias. New York, Alan R Liss Inc. 1982;89-101.
- Nores JM, Dizien O, Remy JM, et al. Two cases of spondylometaphyseal dysplasia. Literature review and
discussion of the genetic inheritance of the disease. J Rheumatol. 1993;20: 170-172.
- Hasegawa T, Kozlowski K, Nishimura G, et al. Japanese type of
spondylometaphyseal dysplasia. Pediatr Radiol. 1994;24: 194-197.
- Marik I, Zemkova D, Baksova A, et al. Spondylo-metaphyseal dysplasia - Kozlowski type. Pol
J Radiol. 2006;71(2): 98-101.
- Sarka C, Jana L, Daniela Z,
et al. Early molecular genetic
diagnosis of spondylometaphyseal dysplasia - Kozlowski type, Locomotor System. 2022;29(1):
133-148.
- Loukin S, Su Z, Kung C. Increased basal activity is a
key determinant in the severity of human skeletal dysplasia caused by TRPV4
mutations. PLoS One. 2011;6: 19533.
- Schmid F. Beitrag zur Dysostosis enchondralis
metaphysarea. Monats Kinderheilkd. 1949;97: 393-397.
- Sutcliffe J, Stanley P. Metaphyseal chondrodysplasias. Prog Pediatr
Radiol. 1973;4: 250-269.
- Murdoch JL, Walker BA. A
"new" form of spondylometaphyseal dysplasia. Birth Defects Orig Art
Serv. 1969;4: 368-370.
- Borochowitz Z, Berant M, Kristal H. Spondylometaphyseal dysplasia:
further heterogeneity. Skeletal Radiol. 1988;17: 181-186.
- Wiedemann
HR, Spranger J. Chondrodysplasia metaphysaria (Dysostosis metaphysaria) - ein
neuer Typ ?. Z Kinderheilkd. 1970;108: 171-186.
- Krakow D,
Vriens J, Camacho N, et al. Mutations
in the gene encoding the calcium-permeable ion channel TRPV4 produce
spondylometaphyseal dysplasia, Kozlowski type and metatropic dysplasia. Am J
Hum Genet. 2009;84: 307-315.
- Genevieve D, Le Merrer M, Feingold J, et al. Revisiting metatropic
dysplasia: presentation of a series of 19 novel patients and review of the
literature. Am J Med Genet. 2008;146: 992-996.
- Dai J, Kim
OH, Cho TJ, et al. Novel and recurrent TRPV4
mutations and their association with distinct phenotypes within the TRPV4
dysplasia family. J Med Genet. 2010;47: 704-709.
- Bhargava R, Leonard NJ, Chan AKJ, et al. Autosomal dominant inheritance
of spondyloenchondrodysplasia. Am J Med Genet. 2005;135: 282-288.
- Dyggve HV, Melchior JC, Clausen J. Morquio-Ullrich's disease. An inborn
error of metabolism? Arch Dis Child. 1962;37: 525-534.
- Kitoh H,
Kaneko H, Kondo M, et al. Spondylometaphyseal
dysplasia with cone-rod dystrophy. Am J Med Genet. 2011;155: 845-849.
- Nishimura
G, Dai J, Lausch E, et al. Spondylo-epiphyseal
dysplasia, Maroteau type [pseudo-Morquio syndrome type 2] and parastremmatic
dysplasia are caused by TRPV4 mutations. Am J Med Genet. 2010;152: 1443-1449.
- Bass HN. London
Dysmorphology Database, London Neurogenetics Database & Dysmorphology Photo
Library on CD-ROM. Am J
Hum Genet. 2002;71(3): 687.
- Weinstein J, Kuo K, Millar E. Congenital coxa vara: a
retrospective review. J Pediatr Orthop. 1984;4: 70-77.
- Unni KK: Cartilaginous
lesions of bone. J Orthop Sci.
2001;6: 457-472.
- Oh CW, Thacker MM, Mackenzie WG, Riddle EC. Coxa vara:
a novel measurement technique in skeletal dysplasias. Clin
Orthop Relat Res. 2006;447: 125-131.
- Chung SM, Riser WH: The histological characteristics of congenital coxa vara: a case report of a five-year-old boy. Clin Orthop. 1978;132: 71-81.
- Magu NK, Rohilla R, Singh R, et al. Modified Pauwels' intertrochanteric osteotomy in neglected femoral neck fracture. Clin Orthop Relat Res. 2009;467(4): 1064-1073.