Knowledge, Attitude and Practices Regarding Chronic Complications of Diabetes among Patients with Diabetes in Northeastern Ethiopia, 2024
Abstract
Background: In 2021, diabetes claimed the lives of 6.7 million people and cost the healthcare system at least $966 billion. Diabetic individuals with a poor understanding of the condition had greater risks of hospitalization for diabetes.
Objective: To assess knowledge, attitude and practices regarding chronic complications of diabetes among patients with diabetes in northeastern Ethiopia in 2024.
Methods: A cross-sectional study design was conducted among 350 diabetic patients in northeastern Ethiopia from April 25 to May 25, 2024. A pretested, structured questionnaire was developed from published sources on the same subject area. SPSS version 22 for Windows was used and binary and multivariate logistic regressions were applied to assess the knowledge, attitude and practice of respondents about diabetic complications. P ≤ 0.05 was used to declare statistically significant variables.
Result: A total of 350 diabetes patients were enrolled, with a response rate of 95%. In this study, 184(58%) of the participants had good knowledge, 188 (59.1%) had a good attitude and 168 (53.4%) had good practice. Patients staying with the disease for more than 10 years were 2.05 times (AOR = 2.05, 95% CI = 1.03, 4.05) more likely to have a good attitude. Government workers were 3.17 times (AOR = 3.17, 95% CI = 1.17, 8.62) more likely to have a good attitude toward chronic complications of DM. Male patients were 1.71 times (AOR = 1.71, 95% CI = 1.10, 2.65) more likely to have good practice than their female counterparts. Patients with a monthly income of 500–1500 and 150–1500 ETB were 2.02 times and 1.97 times more likely to have good practice for chronic complications of DM as compared to patients with a monthly income of < 500 ETB.
Conclusion: Participants with better educational status and a family history of DM were more likely to have good knowledge about diabetic complications. Study subjects with disease duration of more than 10 years and government employees had a positive attitude. Male patients and those with a good monthly income had good practices towards the chronic complications of DM.
Keywords: Attitude, Diabetes mellitus, Knowledge, Practice,
1. Introduction
Diabetes
mellitus (DM) is a severe chronic illness that develops when a patient's serum
glucose levels are high due to either insufficient or no insulin production by
their body or an inability to utilize the insulin that is produced1. Diabetes
mellitus is a complex disease resulting in issues such as population health
decline and increased health-care expenses2. Diabetes is one of the four non-communicable diseases
(NCDs) that the World Health Organization has prioritized for prevention and
control3.
According to the
International Diabetes Federation (IDF) 2021 report, there is
a continued global increase in diabetes prevalence, confirming diabetes as a
significant global challenge to the health and well-being of individuals.
Globally, 537 million adults are living with
diabetes, which is predicted to rise to 643 million by 2030. Moreover, with an
expected 1.5 million fatalities due to diabetes directly in 2019, diabetes
ranked as the ninth most common cause of death1.
It is estimated
that 24 million adults in Africa are living with diabetes and over 1 in 2
people living with diabetes in Africa are not diagnosed. Furthermore,
more than two-thirds of diabetes mellitus patients in Sub-Saharan Africa are
untreated4.
According to an IDF report, diabetes mellitus was present in 3.3% of
Ethiopians5. Other evidence suggests
that the prevalence of diabetes in Ethiopia ranges from 0.5 percent to 6.5
percent6-9.
Diabetes
is linked to significant financial burdens for individuals, families and the
community. Patients with diabetes who experience both macro and microvascular
complications can spend up to 2.5 times as much on care overall as those
without problems10,11. Treatment of comorbidities associated with diabetes is essential
for the patients’ health related quality of life. Over the past few years, the
expense of treating diabetes and associated complications has increased12.
In
addition to preserving an ideal blood glucose level, the aim of diabetes
management is to avoid consequences from the condition, including retinopathy,
neuropathy, nephropathy and cardio cerebrovascular disease13. Non-adherence, a
negative attitude toward the illness and its complications and unhealthy diet
are typical causes of poor diabetic control and hence diabetic complications.
These complications can predispose the patient to different infections and death or disability as final
outcome14. In a US sample of 12,379 participants, hospitalization for
infection-related reasons was much more likely in those with diabetes mellitus
(1.67 times higher) than in those without the condition15.
Sub optimal glycemic management in clinical
practice is linked to diabetes complications such as diabetic ketoacidosis,
micro- and macro-vascular diabetic problems and their associated poor
consequences16. Poor glycemic control
and consequences such as diabetic nephropathy, diabetic retinopathy and
diabetic neuropathy are linked to insufficient diabetes education and self-care
behaviors17. Each 1% drop in mean glycated hemoglobin (HbA1c) has been linked
to a 21% reduction in the risk of diabetes-related mortality, a 14% reduction
in the risk of myocardial infarction and a 37% reduction in the risk of
micro-vascular complications18,19.
With an expected 1.5 million fatalities directly related to
diabetes in 2019, diabetes ranked tenth among all causes of mortality1. Furthermore, those with diabetes are two to three times more
likely to die from any cause, including liver disease, cancer, heart disease,
stroke and chronic renal illness20,21. According to a Chinese study, 76.4% of diabetes patients
reported experiencing at least one type of diabetes related complications22,23. In sub-Saharan Africa, up to 48% of diabetics had neuropathy
symptoms, while 14-18% of diabetics had ocular problems, 10% to 15% of
diabetics have acquired diabetic foot ulcers at some point in their lives and
in sub-Saharan Africa, diabetic foot issues account for over 50% of all
DM-related hospitalizations23. According to a prior study conducted in Ethiopia, 29.4% of
diabetics suffer at least one chronic problem24.
Individuals
diagnosed with diabetes mellitus must keep an eye on their health, specifically
on complications, treatment and prescription schedules. Along with exercise,
diet and medication adjustment, therapeutic adherence is crucial for achieving
glycemic control and preventing complications25-28.
Misconceptions stemming from a lack of awareness, when combined with
insufficient knowledge, are significant obstacles to appropriate diabetes
management29.
Diabetes
self-care routines are significantly influenced by perceptions of sickness and
diabetes knowledge. Furthermore, decision-making about nutrition, exercise,
medication use and health status monitoring which includes diabetic screening
and foot care is influenced by knowledge about the disease30. Diabetic individuals with a poor
understanding of the condition had greater risks of hospitalization for
diabetes, which is unstable31.
Glycemic control knowledge can assist people in comprehending
the risks of diabetes and motivating them to seek appropriate therapy and care
in order to keep the disease under control16. In order to
effectively manage the condition, an individual must be aware of and
knowledgeable about the disease's nature and consequences, as well as its risk
factors, management and chronic complications. The aim of this study was to
assess knowledge, attitude and practices regarding chronic complications of
diabetes among patients with diabetes in a comprehensive specialized hospital
in Woldia, Ethiopia in 2024.
2. Methods
2.1. Study design, period and area
A cross-sectional study design was conducted in Woldia comprehensive specialized hospital from April 25 to May 25, 2024, Woldia, northeast Ethiopia. Woldia Comprehensive Specialized Hospital, located in Woldia Town in Ethiopia, is a prominent healthcare institution dedicated to providing high-quality medical services. As a comprehensive specialized hospital, it serves as a critical healthcare provider for the region, offering a wide range of medical services and specialized treatments to the local population.
2.2. Population
2.2.1.
Source population: All diabetes patients who visited to Woldia comprehensive specialized hospital diabetic clinic.
2.2.2.
Study population: all diabetes patients who fulfill the eligibility criteria and
visited woldia
comprehensive specialized hospital during the data collection time.
2.3. Inclusion
criteria
Diabetic
patients who are on follow up or take regular medical checkups
and services, at Woldia comprehensive specialized hospital diabetic clinic.
Diabetic
patients whose age is greater than 18 years.
2.4. Exclusion
criteria
Diabetics
secondary to pregnancy (gestational DM).
Those unable to respond because of dementia or psychiatric illness. Diabetes
patients admitted to ward
2.5. Sample size
and sampling technique
The convenience
sampling technique was employed to select participants who visited the diabetic
clinic of Woldia Comprehensive Specialized Hospital for routine appointment
visits. So, using this sampling technique, 368 subjects were
recruited. The sample size was calculated using a single population proportion
formula and determined by taking 58.8% as the rate of prevalence (p) of
knowledge toward diabetic complications among diabetics in Gondar, Ethiopia (32),
a 95% confidence level (Zα/2 = 1.96) and a 5% margin of error.
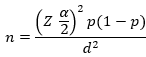
Zα/2 is the standard normal variable value at
(1-α) % confidence level (α is 0.05 with 95% CI, Zα/2 = 1.96),
an estimate of the proportion (p)
was considered as 58.8 % and margin of error (d) 5%.
2.6. Variables
2.6.1. Dependent variables: knowledge, attitude and practice
towards chronic complications of DM.
2.6.2. Independent variables: age, sex, residency, marital status,
occupation, educational status, income, duration since diagnosis as diabetic,
family history and type of DM.
2.7.
Operational definitions
· Diabetes
complications: Acute and chronic
conditions caused by diabetes7.
· Positive attitude: if participants scored ≥ mean score of
answered questions for attitude of diabetic complications
· Poor attitude: if participants scored < mean score of questions about diabetic complications
· Good knowledge: if participants scored ≥ mean score of the correctly answered questions for knowledge
of diabetic complications
· Poor knowledge: participants scored <mean score of the correctly answered questions for knowledge
of diabetic complications
· Good practice: if participants scored ≥ mean score for answers to practice questions about diabetic
complications
· Poor practice: if participants scored < mean score for answers to practice questions about diabetic complications33.
2.8. Data collection tool and data collection process
An organized, pretested interviewer-administered questionnaire was
utilized to collect data regarding knowledge, attitude, practice and associated
factors. A number of published articles were reviewed in order to build the
tool for gathering data34-36. The data collection survey was structured into four primary
sections: Socio-demographic data, diabetes knowledge and history, attitude and
practice-specific data. To ensure consistency in wording, the questionnaire was
produced in English, translated into the local language (Amharic) and then
translated back into English. To calculate the knowledge, attitude and practice
(KAP) score, a scoring system was prepared. Each correct answer was coded as 1,
while each incorrect answer was coded as 0. The data collectors were trained in
the data collection tool before data collection. Each participant was
interviewed face-to-face by a data collection team. The collected data was
checked every day for consistency and completeness before processing.
During data gathering, three trained health professionals were recruited and
supervised by two MSc graduate health professionals.
2.8.1. Assessment of knowledge: The participants had
two options for responses to questions testing their knowledge of diabetes
complications: "Yes" or "No." A "0" point was
given for no and a "1" point for yes. After calculating the mean
knowledge score, knowledge was divided into two categories: good and poor.
Participants were classified as having good knowledge if their answers scored higher
than the mean (10.6) and as having poor knowledge if their answers scored lower
than the mean (10.6).
2.8.2. Assessment of attitude: To assess the patients' attitudes,
we had adapted questions from several articles. There were three options for
each question: agree, neutral and disagree. For each attitude question, a score
of "0" indicated an unfavorable attitude (disagree and indifferent),
while a score of "1" indicated a favorable attitude (right answer).
By adding up the correct responses and computing the mean value, the diabetic
patient's attitude toward complications related to their diabetes was
determined. Individuals who scored lower than the average (22.9) were
classified as having negative attitudes. Those who scored higher than the
average (22.9) was considered to have a positive attitude.
2.8.3.
Assessment of practice
Patients
were asked questions about diabetic complications and were asked to respond
with a "Yes" or "No." "Yes" receives a score of
1, while "No" receives a score of 0. "Yes" indicates that
the patient is adhering to the advised course of action. Subsequently, Then,
the patient’s practice level was calculated by adding their responses and
calculating the mean which is 7.9. Those with a mean score or higher were
considered good practice while the remaining scores were classified as poor
practice.
2.9. Data processing and analysis
The social science statistics package (SPSS) version 22 for Windows was used to enter the gathered data. The mean (± SD) was used to express all continuous data, while numbers and percentages were used to express categorical variables. Descriptive statistics and frequency distributions were used to describe participant characteristics. Based on bi-variable analysis, variables with a p-value < 0.25 were entered into a multivariable logistic regression model; P ≤ 0.05 was used to declare statistically significant variables in the final model. Descriptive statistics, such as frequencies and percentages, were used. A binary logistic regression was used to identify predictors of awareness of diabetes and its complications.
2.10. Data quality control
The principal investigator performed continuous oversight and follow-up to ensure the quality of the data. In addition, the data was checked on a daily basis for completeness and consistency and then corrections were made accordingly.
2.11. Ethical approval
Ethical approval was obtained from Woldia comprehensive specialized hospital ethical review committee with ethical clearance number ERC 016/2024. A permission letter was obtained from the medical director's office. Written consent was obtained from each respondent in the study to fulfill ethical considerations and confidentiality was maintained throughout the study process.
3. Result
A
total of 350 diabetes
patients were enrolled, with a response rate of 95%.
3.1. Socio-demographic characteristics of respondents
Out of 350 diabetic respondents, 178 (50.9%)
were male and 172 (49.1%) were female. The majority of participants were
Orthodox Christian followers
(66%).
Concerning to educational status, 156(44.5%) study participants were Secondary school and above. Approximately 30% of the population earned more than 2500 ETB a month. About 60.6% of participants were urban dwellers and 48.9% had had diabetes for one to five years (Table 1). Around half of
participants 171(48.9%) were under oral hypoglycemic treatment.
Table 1: Socio-medical characteristics of study participants in WCSH, 2024.
|
Variables |
Categories |
Frequency |
Percent (%) |
|
Sex |
Male |
178 |
50.9 |
|
|
Female |
172 |
49.1 |
|
Educational status |
No formal education |
108 |
30.9 |
|
|
Primary |
86 |
24.6 |
|
|
Secondary and above |
156 |
44.5 |
|
Marital status |
Single |
62 |
17.7 |
|
|
Married |
210 |
60 |
|
|
Widowed |
13 |
3.7 |
|
|
Divorced |
65 |
18.6 |
|
Religion |
Orthodox |
231 |
66 |
|
|
Muslim |
101 |
28.9 |
|
|
Protestant |
18 |
5.1 |
|
Residence |
Urban |
212 |
60.6 |
|
|
Rural |
138 |
39.4 |
|
Duration of diseases |
1-5 |
171 |
48.9 |
|
|
6-10 |
119 |
34 |
|
|
>10 |
60 |
17.1 |
|
Type of medication |
Oral |
171 |
48.9 |
|
|
Injectable |
166 |
47.4 |
|
|
Both |
13 |
3.7 |
|
Family history of DM |
No |
177 |
50.6 |
|
|
Yes |
173 |
49.4 |
|
Monthly income |
<500 |
66 |
18.9 |
|
|
500-1500 |
91 |
26 |
|
|
1501-2500 |
88 |
25.1 |
|
|
>2500 |
105 |
30 |
3.2. Knowledge,
attitude and practice
In this study, 184 (58%) of the participants had good knowledge, 188 (59.1%) had a good attitude and 168 (53.4%) had good practice (Figure 1).
Figure 1: KAP regarding chronic
complication of diabetes among patients with diabete in WCSH, 2024.
3.3.
Factors associated with good knowledge
In
multivariable analysis, education status, religion and family history of DM
were significantly associated with good knowledge of chronic complications of
diabetes. Patients who had primary education were 56% (AOR = 0.44, 95% CI =
0.23, 0.85) less likely to have good knowledge as compared to those who attended
secondary education and above. Regarding religion, protestant patients were 82%
(AOR = 0.18, 95% CI = 0.06, 0.55) less likely to have good knowledge (Table
2). Those with a family history of DM were 1.86 times (AOR = 1.86, 95% CI =
1.16, 3.00), more likely to have good knowledge as compared to their
counterparts.
Table 2: Factors associated with knowledge towards chronic diabetic complications of study participants in WCSH, 2024.
|
Variables |
Category |
AOR |
95% CI |
|
Sex |
Female |
1 |
1 |
|
|
Male |
1.21 |
0.71, 2.05 |
|
Occupation |
Unemployed |
1 |
1 |
|
|
Farmer |
0.80 |
0.33, 1.95 |
|
|
Housewife |
1.61 |
0.63, 4.14 |
|
|
Gov’t worker |
1.24 |
0.46, 3.30 |
|
|
Other |
1.75 |
0.69, 4.38 |
|
Education status |
No formal education |
1 |
1 |
|
|
Primary |
0.44 |
0.23, 0.85* |
|
|
Secondary and above |
0.86 |
0.39, 1.90 |
|
Religion |
Orthodox |
1 |
1 |
|
|
Muslim |
1.14 |
0.67, 1.91 |
|
|
Protestant |
0.18 |
0.06, 0.55* |
|
Residence |
Urban |
1 |
1 |
|
|
Rural |
0.72 |
0.39, 1.36 |
|
Family history |
No |
1 |
1 |
|
|
Yes |
1.86 |
1.16, 3.00* |
|
Income |
< 500 |
1 |
1 |
|
|
500 – 1500 |
0.88 |
0.40, 1.94 |
|
|
1501-2500 |
0.47 |
0.21, 1.04 |
|
|
> 2500 |
1.06 |
0.41, 2.72 |
3.4.
Factors associated with attitude
Factors
such as residence, duration of diseases, occupational status and level of
knowledge were significantly associated with the attitude of respondents.
Regarding
the duration of diseases, those patients staying with the disease for more than
10 years were 2.05 times (AOR = 2.05, 95% CI = 1.03-4.05) more likely to have a
good attitude towards chronic complications of diabetes as compared to the
counterparts, while the effect of other variables kept constant. The other
significant predictor was occupation and patients who are government workers
were 3.17 times (AOR = 3.17, 95% CI = 1.17, 8.62) more likely to have a good
attitude toward chronic complications of DM (Table 3).
Table 3: Factors associated with attitude towards chronic diabetic complications of study participants in WCSH, 2024.
|
Variables |
Category |
AOR |
95% CI |
|
Residence |
Urban |
1 |
1 |
|
|
Rural |
0.49 |
0.27,0.91* |
|
Duration of diseases in
years |
1-5 |
1 |
1 |
|
|
6-10 |
0.89 |
0.52, 1.51 |
|
|
>10 |
2.05 |
1.03, 4.05* |
|
Monthly income |
< 500 |
1 |
1 |
|
|
500 – 1500 |
1.40 |
0.63, 3.11 |
|
|
1501-2500 |
0.69 |
0.32, 1.52 |
|
|
> 2500 |
0.60 |
0.25, 1.47 |
|
Occupation |
Unemployed |
1 |
1 |
|
|
Farmer |
1.16 |
0.53, 2.56 |
|
|
Housewife |
1.14 |
0.50, 2.61 |
|
|
Gov’t worker |
3.17 |
1.17, 8.62* |
|
|
Others |
1.36 |
0.57, 3.21 |
|
Level of knowledge |
Poor |
1 |
1 |
|
|
Good |
2.47 |
1.55, 3.95 |
3.5.
Determinants of good practice towards chronic complications of DM
In
multivariable analysis, sex and income of patients were significantly
associated with practice toward chronic complications of DM. As compared to
female patients, male patients were 1.7 times more likely to have good practice
(AOR = 1.71, 95% CI = 1.10, 2.65) (Table 4). Those patients with a
monthly income of 500-1500 and 150-1500 were 2.02 times (AOR = 2.02, 95% CI =
1.05-3.88) and 1.97 times (AOR = 1.97, 95% CI = 1.02-3.81) more likely to have
good practice for chronic complications of DM as compared to patients with a
monthly income of < 500 birr.
Table 4: Factors associated with practice towards chronic diabetic complications of study participants in WCSH, 2024
|
Variables |
Category |
AOR |
95 % CI |
|
Sex
|
Female
|
1 |
1 |
|
|
Male
|
1.71 |
1.10,
2.65* |
|
Religion
|
Orthodox
|
1 |
1 |
|
|
Muslim
|
0.73 |
0.45,
1.18 |
|
|
Protestant
|
1.67 |
0.59,
4.72 |
|
Income
|
< 500 |
1 |
1 |
|
|
500
- 1500 |
2.02 |
1.05,
3.88* |
|
|
1501-2500 |
1.97 |
1.02,
3.81* |
|
|
>
2500 |
1.45 |
0.76,
2.76 |
4. Discussion
Worldwide, diabetes is one of the leading
causes of death36. It is a chronic illness with a variety of complications that
require in-depth understanding and care. Adequate knowledge of DM and its
complications is necessary for diabetes self-management37.
In this study,
184 (58%) of the participants had good knowledge. This is in line with results from Ethiopia (59%)38, Malaysia (58.1%)39, Tarlai 57%40, India (50.1%)41, Debre Tabor (Ethiopia) (51%). And this finding is
higher than reports from a study in Ghana, which reported
45.9 % of participants had good knowledge of diabetes complications42. However, the findings of our study
are incomparable with those of a Saudi Arabian study, which reported that 80%
of participants knew the complications associated with diabetes and a study
from Nigeria, where 90.5% of type 2 DM patients had adequate knowledge of
diabetes complications43. Variations
in socioeconomic conditions, cultural beliefs and behaviors may account for the
discrepancy, as they have an effect on the pattern of awareness regarding
diabetic consequences44.
The results of this study showed a
favorable association between participants' knowledge of diabetic complications
and their educational status. This is supported by other study findings that
reported a positive relationship between the level of education and the degree
of knowledge about diabetic complications42,45-48. The knowledge of diabetics about maintaining appropriate
blood glucose levels was greatly influenced by education49. Knowledge is one of the predictors of behavior in
many ways50. This might be due to increased opportunity
of learning about DM
complications from various sources as they become more knowledgeable.
Furthermore, educated people have access to a variety of medical literatures44.
Respondents
with family history of DM were 1.86 times more likely to have good knowledge
about diabetic complications as compared to their counterparts. This is
consistent with findings from the study done in India44,47 and Ethiopia44. Receiving
information from the family with chronic disease might influence the patient’s
attitude and daily practice, which can be a good source of information51. This is as a result
of their learning from family experiences.
In this study,
about 59.1%
of study participants had a good attitude. This is in contrast to the results
of a study done in Ethiopia, in which over 65.2% of the study participants had
a good attitude level35. Differences in culture and socioeconomic status could be the
explanation. Our study findings revealed that, regarding the duration of
diseases, those patients staying with the diseases for more than 10 years were
2.05 times more likely to have a good attitude towards chronic complications of
diabetes as compared to the counterparts when the effect of other variables
kept constant. This is supported by findings from a recent study conducted in
Iran, which reported a substantial positive link between attitude level and the
length of the disease51.
The
other significant predictor in this study was occupation. Patients who are
government workers were 3.17 times more likely to have a good attitude toward
chronic complications of DM. This is supported by a study from southeast
Ethiopia which reported that employment in the public or private sector was
three times more likely to result in a favorable attitude toward DM33. This might be due to
patients with greater education and employment status may find it easier to
obtain and read various resources and they may also be able to speak with
medical staffs without difficulty. This aids in their knowledge gathering and
helps them adopt a more positive outlook regarding DM complications35,52.
Regarding practice, as compared to female patients, male patients were 1.71 times more
likely to have good practice. This is in line with a study from Bangladesh
which reported higher level of practice among males than
females36. Those patients with a monthly income of 500-2500 birr were 2.02
times more likely to have good practice for chronic complications of DM as
compared to patients with a monthly income of < 500 birr. Low income
is associated with poor access to educational opportunities regarding methods
of preventions of diabetes. This could also be because people with lower
incomes would have to wait longer to get health care53.
5. Limitation
Since the information about the attitudes and practices
related to DM problems was self-reported, recall bias might have existed. The study was conducted on all diabetic patients regardless
of their diabetic complication history status during the data collection period
which could possibly affect knowledge, attitude and practice levels. And being
cross-sectional study, this study did not show the conditions of cause-and-effect
relationships.
6.
Conclusion
A higher percentage of diabetes patients had generally
positive attitude, knowledge and practice towards preventing diabetic
complications in this study. Participants with better educational status and having
family history of DM were more likely to have good knowledge about diabetic
complications. Study subjects with disease duration more than 10 years with
diabetes and government employees were more likely to have positive attitude
towards chronic complications of diabetes. Male patients and those with a
monthly income of 500 -2500 ETB had good practice to prevent chronic
complication of DM as compared to patients with monthly income of < 500 ETB. Based on the above information,
increasing health education about diabetic complication will help to maintain
the good KAP of the population and fills gaps in prevention.
7.
Abbreviations and Acronyms
AOR- adjusted odds ratio
CI- confidence interval
CVD- cardiovascular diseases
DM- diabetes mellitus
ETB- Ethiopian birr
NCDS- Non communicable diseases
IDF- International diabets federation
SPSS- statstical packages for social sciences
WSCH- woldia specialized comprehensive hospital
8.
Declarations
8.1. Ethical approval
Ethical
approval was obtained from Woldia comprehensive specialized hospital ethical
review committee with ethical clearance number ERC 016/2024. Written consent was obtained from each respondent in the study
to fulfill ethical considerations and confidentiality was maintained throughout
the study process.
8.2. Consent for
publication
Not applicable.
8.3. Data
availability
The data used in this study
are included and available in the whole manuscript. The dataset can be
available at the hand of the corresponding author and can be accessed upon
reasonable request.
8.4. Competing
interest
All authors
declared that there is no competing interest.
8.5. Authors' contributions
All authors have contributed equally for the manuscript.
8.6. Funding
Not applicable.
8.7. Acknowledgment
We thank all participants and
facilitators from for their support in accomplishment of this study.
9. References
- Roth G. Global Burden of Disease
Collaborative Network. Global Burden of Disease Study 2017 (GBD 2017) Results.
Seattle, United States: Institute for Health Metrics and Evaluation (IHME),
2018. The Lancet, 2018;392: 1736-1788.
- Bickler SW, Wang A, Amin S, et al. Urbanization in
Sub-Saharan Africa: Declining Rates of Chronic and Recurrent Infection and
Their Possible Role in the Origins of Non-communicable Diseases. World J Surg,
2018;42: 1617-1628.
- Organization WHO.
Noncommunicable diseases country profiles CC BY-NC-SA 3.0 IGO, 2018.
- James SL, Abate D, Abate KH, et al. Global, regional
and national incidence, prevalence and years lived with disability for 354
diseases and injuries for 195 countries and territories, 1990–2017:
a systematic analysis for the Global Burden of Disease Study 2017. The Lancet,
2018;392: 1789-1858.
- Bekele BB. The prevalence of macro and microvascular
complications of DM among patients in Ethiopia 1990-2017: Systematic review.
Diabetes & Metabolic Syndrome: Clin Res Reviews, 2019;13: 672-677.
- Endriyas M,
Mekonnen E, Dana T, et al. Burden of NCDs in SNNP region, Ethiopia: a retrospective
study. BMC Health Services Research, 2018;18: 520.
- Gizaw M, Harries AD, Ade S, et al. Diabetes mellitus
in Addis Ababa, Ethiopia: admissions, complications and outcomes in a large
referral hospital. Public Health Action, 2015;5: 74-78.
- Tesfaye T, Shikur B, Shimels T,
et al. Prevalence and factors associated with diabetes mellitus and impaired
fasting glucose level among members of federal police commission residing in
Addis Ababa, Ethiopia. BMC Endocrine Disorders, 2016;16: 68.
- Abebe SM, andargie G, Shimeka A, et al. The
prevalence of non-communicable diseases in northwest Ethiopia: survey of Dabat
Health and Demographic Surveillance System. BMJ Open, 2017;7: e015496.
- Schofield D, Cunich MM, Shrestha
RN, et al. The economic impact of diabetes through lost labour force
participation on individuals and government: evidence from a microsimulation
model. BMC public health, 2014;14: 1-8.
- Susan van D, Beulens JW, Yvonne T. van der S, et al.
The global burden of diabetes and its complications: an emerging pandemic.
European J Cardiovascular Prevention Rehab, 2010;17: s3-s8.
- Bannier K,
Lichtenauer M, Franz M, et al. Impact of diabetes mellitus and its complications: survival
and quality-of-life in critically ill patients. Journal of diabetes and its
complications, 2015;29: 1130-1135.
- Association AD. 6. Glycemic
targets: standards of medical care in diabetes-2018. Diabetes care, 2018;41: S55-S64.
- Abejew AA, Belay AZ, Kerie MW.
Diabetic complications among adult diabetic patients of a tertiary hospital in
northeast Ethiopia. Advances in Public Health, 2015;2015: 290920.
- Tomic D, Shaw JE, Magliano DJ.
The burden and risks of emerging complications of diabetes mellitus. Nature
Reviews Endocrinology, 2022;18: 525-539.
- Asmelash D, Abdu N, Tefera S, et al. Knowledge,
Attitude and Practice towards Glycemic Control and Its Associated Factors among
Diabetes Mellitus Patients. Journal of Diabetes Research. 2019;2019: 2593684.
- Fasil A, Biadgo B, Abebe M. Glycemic control and
diabetes complications among diabetes mellitus patients attending at University
of Gondar Hospital, Northwest Ethiopia. Diabetes Metab Syndr Obes, 2018;12: 75-83.
- Kibirige D AG, Kampiire L,
Kiggundu DS, et al. Frequency and predictors of suboptimal glycemic control in
an African diabetic population. Int J Gen Med, 2017;10: 33-38.
- Atlas ID. Diabetes around the
world in 2021.
- Yang JJ, Yu D, Wen W, et al.
Association of diabetes with all-cause and cause-specific mortality in Asia: a
pooled analysis of more than 1 million participants. JAMA network open, 2019;2:
192696.
- Bragg F, Holmes MV, Iona A, et al. Association
between diabetes and cause-specific mortality in rural and urban areas of
China. Jama, 2017;317: 280-289.
- Mao WenHui MW, ChiMan Y, Chen
Wen CW. Complications of diabetes in China: health system and economic
implications, 2019.
- Sarpong C, Nsiah K, Mensah F, et
al. Prevalence of the Complications of Diabetes in Developing countries.
Archives of Clin Biomed Res, 2017;1: 235-241.
- Ahmed M, Yirdachew E, Tefera G.
Diabetic complications among follow-up patients: a cross-sectional study at
Jimma University specialized hospital diabetic clinic. J Clin Mol
Endocrinol, 2018;3: 45.
- Gregório
MJ, Sousa Sd, Ferreira B, et al. Programa Nacional para a Promoção da
Alimentação Saudável 2020.
- ElSayed NA, Aleppo G, Aroda VR,
et al. Glycemic targets: standards of care in diabetes-2023. Diabetes care,
2023;46: S97-S110.
- Mirahmadizadeh A, Khorshidsavar H, Seif M, et al.
Adherence to medication, diet and physical activity and the associated factors
amongst patients with type 2 diabetes. Diabetes Therapy, 2020;11: 479-494.
- Saleh AM. People with diabetes adherence to drug,
dietary and lifestyle changes in Erbil city, Iraq. BMC Endocrine Disorders,
2022;22: 305.
- Alemayehu AM, Dagne H, Dagnew B. Knowledge and
associated factors towards diabetes mellitus among adult non-diabetic community
members of Gondar city, Ethiopia 2019. PloS one, 2020;15: e0230880.
- Kumar R,
Itumalla R, Perera B, et al. Patient knowledge about diabetes: Illness symptoms,
complications and preventive personal lifestyle factors. Health Psycho Res,
2022;10.
- Abdullah L, Margolis S, Townsend T. Primary health
care patients' knowledge about diabetes in the United Arab Emirates, 2001.
- Berihun G, Walle Z, Berhanu L, et al. Acceptance of
COVID-19 vaccine and determinant factors among patients with chronic disease
visiting Dessie Comprehensive Specialized Hospital, Northeastern Ethiopia.
Patient preference and adherence, 2021: 1795-1805.
- Kassahun CW, Mekonen AG. Knowledge, attitude,
practices and their associated factors towards diabetes mellitus among non
diabetes community members of Bale Zone administrative towns, South East
Ethiopia. A cross-sectional study. PloS one, 2017;12: e0170040.
- Kifle ZD,
Adugna M, Awgichew A, et al. Knowledge towards diabetes and its chronic complications and
associated factors among diabetes patients in University of Gondar
comprehensive and specialized hospital, Gondar, Northwest Ethiopia. Clinical
Epidemiology and Global Health, 2022;15: 101033.
- Belsti Y, Akalu Y, Animut Y.
Attitude, practice and its associated factors towards Diabetes complications
among type 2 diabetic patients at Addis Zemen District hospital, Northwest
Ethiopia. BMC Public Health, 2020;20: 1-11.
- Rahaman KS, Majdzadeh R, Naieni
KH, et al. Knowledge, attitude and practices (KAP) regarding chronic
complications of diabetes among patients with type 2 diabetes in Dhaka.
International journal of endocrinology and metabolism, 2017;15.
- Gautam A, Bhatta DN, Aryal UR.
Diabetes related health knowledge, attitude and practice among diabetic
patients in Nepal. BMC endocrine disorders, 2015;15: 1-8.
- Gizaw A, Belachew Y, Kebede D.
Knowledge about Dia-betic complications among patients on diabetic follow up
Clinic at Jimma Uni-versity Medical Centre; 2019. J Diabetes Metab Disord.
2019;6:029.
- Minhat H, Hamedon T. Understanding towards diabetes
mellitus among rural adult community in Malaysia. World J Med Sci, 2014;11: 217-221.
- Ulvi OS, Chaudhary RY, Ali T, et al. Investigating
the awareness level about diabetes mellitus and associated factors in Tarlai
(rural Islamabad). JPMA The Journal of the Pakistan Medical Association,
2009;59: 798-801.
- Rani PK, Raman R, Subramani S, et al. Knowledge of
diabetes and diabetic retinopathy among rural populations in India and the
influence of knowledge of diabetic retinopathy on attitude and practice. Rural
and remote health, 2008;8: 1-9.
- Afaya RA, Bam V, Azongo TB, et al. Knowledge of
chronic complications of diabetes among persons living with type 2 diabetes
mellitus in northern Ghana. Plos one, 2020;15: 0241424.
- Adeyemi O, Timothy T,
Oluwanimodimu D, et al. Knowledge of Diabetic Complications and Practice of
Routine Medical Check-up among Type 2 Diabetics in Nigeria. Journal of Advances
in Medicine and Medical Research, 2018;25: 1-8.
- Belsti Y, Akalu Y, Fekadu H, et
al. Awareness of complications of diabetes mellitus and its associated factors
among type 2 diabetic patients at Addis Zemen District Hospital, northwest
Ethiopia. BMC Research Notes, 2019;12: 1-7.
- Obirikorang
Y, Obirikorang C, Anto EO, et al. Knowledge of complications of diabetes mellitus among
patients visiting the diabetes clinic at Sampa Government Hospital, Ghana: a
descriptive study. BMC public health, 2016;16: 1-8.
- Ullah F, Afridi AK, Rahim F, et al. Knowledge of
diabetic complications in patients with diabetes mellitus. Journal of Ayub
Medical College Abbottabad, 2015;27: 360-363.
- Murugesan N, Snehalatha C, Shobhana R, et al.
Awareness about diabetes and its complications in the general and diabetic
population in a city in southern India. Diabetes research and clinical practice,
2007;77: 433-437.
- Nisar N, Khan IA, Qadri MH, et
al. Knowledge and risk assessment of diabetes mellitus at primary care level: a
preventive approach required combating the disease in a developing country. Pak
J Med Sci, 2008;24: 667-672.
- Hoque MA, Islam MS, Khan MAM, et
al. Knowledge of diabetic complications in a diabetic population. Journal of
Medicine, 2009;10: 90.
- Albarracín D, Johnson BT, Zanna
MP. The handbook of attitudes: Psychology Press, 2014.
- Niroomand
M, Ghasemi SN, Karimi-Sari H, et al. Diabetes knowledge, attitude and practice (KAP) study
among Iranian in-patients with type-2 diabetes: a cross-sectional study.
Diabetes & Metabolic Syndrome: Clinical Research & Reviews, 2016;10: 114.
- Alaofè H, Hounkpatin WA, Djrolo F, Ehiri J, et al. Knowledge, attitude, practice and associated factors among patients with type 2 diabetes in Cotonou, Southern Benin. BMC Public Health, 2021;21: 1-11.
- Kidanie BB, Alem G, Zeleke H, et
al. Determinants of diabetic complication among adult diabetic patients in
Debre Markos referral hospital, northwest Ethiopia, 2018: unmatched case
control study. Diabetes, Metabolic Syndrome and Obesity, 2020: 237-245.
Appendix
Tool for
assessing KAP towards chronic complications of diabetes among diabetic patients
at northeast Ethiopia, 2023.
Questions for
assessing socio demographic conditions
Questions for assessing Knowledge towards chronic complications of diabetes
|
Variables |
Yes |
No |
|
DM is a condition of insufficient insulin production |
|
|
|
DM is a condition of a body which not responding
to insulin |
|
|
|
DM is a condition of high level of sugar in
the blood |
|
|
|
DM is not curable |
|
|
|
DM is disease that affects any part of the
body |
|
|
|
What are risk factors of DM |
|
|
|
Older age |
|
|
|
Being overweight |
|
|
|
Family history |
|
|
|
Pregnancy |
|
|
|
Poor dietary habits |
|
|
|
Inadequate exercise |
|
|
|
Sign and symptoms |
|
|
|
Frequent urination |
|
|
|
Excessive thirst |
|
|
|
Excessive hunger |
|
|
|
Weight loss |
|
|
|
High
blood sugar |
|
|
|
Slow healing of cuts |
|
|
|
Blurred vision |
|
|
|
Feeling of weakness |
|
|
|
Control and management of DM |
|
|
|
Insulin injection available for control and
management of DM |
|
|
|
Tablets and capsules are available for
control and management of DM |
|
|
|
Regular exercise |
|
|
|
Practice healthy diet |
|
|
|
Feet and toe medical checkup and care |
|
|
|
Complication of DM |
|
|
|
Diabetes can cause blindness |
|
|
|
Diabetes Can cause kidney failure |
|
|
|
Diabetes can cause heart failure |
|
|
|
Diabetes can cause stroke |
|
|
|
Diabetes can result in amputation of limb |
|
|
Questions for
assessing attitude towards chronic complications of diabetes
|
Variables |
Agree |
Neutral |
Disagree |
|
I don’t mind if others know I am diabetic |
|
|
|
|
Do you think you should be examined for
diabetes |
|
|
|
|
Do you think family members should be
screened for DM |
|
|
|
|
Do you think family support from family and
friends is important in dealing with diabetes |
|
|
|
|
Do you think we should avoid consuming too
much sugar |
|
|
|
|
DM doesn’t seriously affect marital status |
|
|
|
|
I don’ think DM seriously affects daily
activities |
|
|
|
|
Do you think physical activity can prevent
risk of DM |
|
|
|
|
Do you think maintaining healthy weight helps
prevent DM |
|
|
|
|
DM complication can prevented If blood
glucose level is well maintained |
|
|
|
Questions for assessing practice towards chronic complications of diabetes
|
Gender |
Male |
|
|
Female |
|
|
|
Age |
<24 |
|
|
25-34 |
|
|
|
35-44 |
|
|
|
>44 |
|
|
|
Marital status |
Single |
|
|
Married |
|
|
|
Divorced |
|
|
|
Widowed |
|
|
|
Education |
Illiterate |
|
|
Elementary |
|
|
|
Secondary |
|
|
|
College and above |
|
|
|
Occupation |
House wife |
|
|
Merchant |
|
|
|
Farmer |
|
|
|
Gov’t /private
employee |
|
|
|
Daily laborer |
|
|
|
Average family income
|
< 500 ETB |
|
|
500-1000 ETB |
|
|
|
1000-2000 ETB |
|
|
|
>2000 |
|
|
|
Have you heard about
DM? |
Yes No |
|
|
Source of information
about DM |
Media |
|
|
Friends/relatives |
|
|
|
Health care workers |
|
|
|
Others |
|
|
|
Family history DM |
Yes |
|
|
|
Don’t know |
|
|
|
No |
|
|
Variables |
Yes |
No |
|
Consume fatty foods |
|
|
|
Physical activity of 30-60 min daily |
|
|
|
Maintaining your body weight |
|
|
|
Drinking alcohol and smoke tobacco |
|
|
|
Check your blood sugar |
|
|