Amyand’s Hernia: Incidental Finding of Inflamed Appendix as Hernial Sac Content and its Management
Introduction
Inguinal Hernias accounts to be one of the most indicated conditions for the surgeries of Abdomen throughout the world and the contents of the hernial sac usually are omentum and small intestine1. Now, sometimes hernial sac can also contain appendix tissue which is termed as Amyand's Hernia. It is a rare condition characterizing almost 1% of inguinal hernias2.
Amyand's Hernia is a mixture of two most commonly occurring conditions named as Inguinal hernia and appendicitis. Latest data shows its prevalence to be between 0.4-0.6% reaching to 1% in paediatric patients3. It may present with appendicitis alongside in 0.8-0.13% of the cases4. Right sided Amyand's Hernia is more common than left sided due to increased chances of Right Inguinal hernia and appendicitis and normal anatomical location of appendix.
Here we present a case of 6 months old male patient that was surprisingly diagnosed to be a case of Amyand’s hernia, despite having no clinical indications of appendicitis, intra operatively and was managed by appendectomy and herniotomy alongside.
Keywords:
Inguinal hernias; Appendicitis; Swelling; Tachycardia
Case report
Patient had no associated fever, tachycardia or other usual signs and symptoms. Urinary and bowel habits
were unchanged, and no discharge
of any sort was present
from the penis. The patient had no other comorbid or
illnesses and no history of any previous illnesses or surgeries. The immunization history of patient was positive and
according to the EPI guidelines. No
significant family history of hernias, asthma, Tuberculosis, diabetes mellitus, hypertension, thalassemia was noted.
On examination, patient
had low grade fever of 99 degrees
Fahrenheit and high pulse rate of 142
beats per minute. Local genitalia examination revealed tender scrotal region
with a large swelling on the right side. The
swelling was tender, reducible, with normal skin colour and body temperature. The contents of the
swelling had soft consistency. The baby cried during examination.
Patient
was advised following stated labs and investigations and admission to the
surgical ward for preparation for the elective herniotomy at the upcoming
scheduled day of surgery because no urgency for surgery on the examination and
investigations was indicated.
The Clinical Lab Investigations done were:
Complete Blood Count, Prothrombin time (PT), Activated
partial thromboplastin time (aPTT), INR, with all of them being within normal
ranges.
Radiological investigations included Chest X Ray that
was unremarkable and Ultrasound scrotum
which indicated an anechoic fluid surrounding right testes suggestive of
hydrocele and a loop in upper part of
scrotum with intact vascularity. However, that loop had no peristalsis. Both testes were within
scrotal sacs and with uniform parenchymal echotexture. Vascular flow was also intact. This Ultrasound report was one of
the main causes eliminating any
urgency for the surgery as no strangulation or disturbance in the blood supply
was observed. During surgery,
while exploring the hernial sac, an inflamed
appendix of almost
2 inches was found
(Figure 1).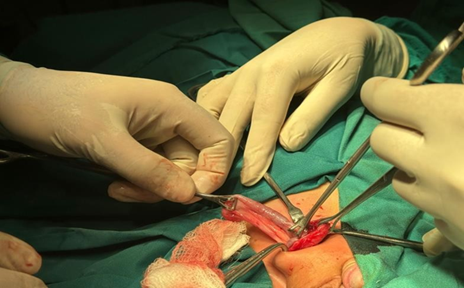
Figure 1: Picture of inflamed appendix
extracted from the hernial sac
This surprising finding was further followed by more
exploration. The appendix was resected, hernial sac was excised and closed.
Internal muscular layers were approximated using vicarly 2-0 suture and skin was closed using Proline
2-0 suture.
Histopathological analysis of the appendicular
specimen showed appendix exhibiting congested
blood vessels and confirmed the acute appendicitis.
Patient was made NPO for 6 hours pre- and post-surgery
and then resumed oral feeding starting
with soft diet and fluids first. Patient was discharged on third post-op day
after keeping under observation in
ward for two days post-op. He followed up along his mother in surgical OPD one week later and
proline-suture-made-skin-stitches were removed after making sure that the surgical site was normal with no signs of
surgical site infection, oozing of blood or
pus.
Discussion
Amyand’s hernia has been ranging in the
literature from 0.19% to 1.7% and the presence of appendicitis, as it was in
our case, along with it is even rarer ranging from 0.07 to 0.13%5.
Its more common in children than in
adults because of the presence
of patent processus vaginalis in children.
The literature indicates that appendix moves into the
hernial sac. The presence of patent processus
vaginalis and an additional connection of appendix with testes favours its
above stated movement and also
supports the cause in our case6.
Leafing further through literature
supported that the increased amount of pressure in the abdomen caused by the abdominal muscles’
contraction aids in the inflammation of the appendix by cutting its blood supply and facilitating the growth of bacteria
inside it7. This reduction in blood supply does not
mean to be completely absent and could only
be slightly reduced
initiating and propagating the process of inflammation passively
as could be here
in this case too because the vascularity in the
ultrasonography was intact.
Usually, the patients that present with Amyand’s
hernia have typical signs and symptoms of appendicitis
and hernia like fever, pain, nausea, chills and skin changes like erythema but here the patient just had complaints of
pain and swelling and a low-grade body temperature not significant enough to be diagnosed as an urgency or a case
of inflammation going on in the
body leading to a misleading diagnosis and ending up with a surprising finding
of inflamed appendix in the hernia.
Management
of the Amyand’s hernia is very well documented and explained according to the type. Losanoff and Basson in 2008,
classified it into four different types along with management of each type8. Type 1 means
hernia having normal
appendix, type 2 explains hernia with acute inflammation of appendix but
without any complications, type 3
means appendicitis with complications like perforation or formation of abscess and type 4 means that there are some other
disease processes that
caused the inflammation and that could be malignancies or conditions like diverticulitis.
The management is also different in the literature for each type of Amyand’s hernia with type 1 being
recommended to be treated with mesh-oriented hernia repair and appendectomy, type 2 being recommended for open
appendectomy without any mesh repair,
type 3 focusing on controlling the acute infection-causing sources and type 4 should be treated specific to the disease
process causing inflammation. In our case it was type 2 and was managed accordingly the guidelines stated in the
literature. The patient underwent
open appendectomy and hernia was repaired without any mesh placement to prevent the infection that could be caused
by the mesh and due to the age of patient further eliminating the need for
any mesh.
Conclusion
Amyand's hernia is not a common finding and that is
why it poses unique diagnostic and management
challenges. The clinical presentation of this patient was very much like an inguinal hernia, but it lacked symptoms
and signs any infection or any Gastrointestinal disturbance. The initial
radiological investigation also suggested a hernia and hydrocele both being
non urgent in nature, but intraoperative finding of inflamed appendix came out
to be a surprise. Its proper
management included appendectomy and herniotomy followed by post operative care. Histopathological analysis also
confirmed that it was acute appendicitis, affirming that surgical intervention was required.
This case shows that though this type of hernia is rare to find, still it
should be kept in mind when diagnosing hernias especially in children even if typical
presentation of appendicitis is not there.
References
1. Rathod JB, Pathak HV, Ajediya KP, Bhatt RK. Amyand’s
Hernia: Incarcerated Appendicitis in a Recurrent
Inguinal Hernia in an Adult. Cureus
2024.
2. Kalayci T, Iliklerden ÜH. Management of incidental amyand
hernia with a case report.
Eastern J Med 2019;24:551-553.
3. Almetaher HA, Mansour
MA, Arafa MA. Management of Amyand’s hernia in children: should appendectomy
be mandatory or not? Annals of Pediatric Surgery
2020;16.
4. Jhanwar P, Rehman S. Amyands hernia in pediatric
case: Manageable but challenging to diagnose preoperatively. IP Inter J Medical Paediatric Onco 2023;9.
5. Ivashchuk G, Cesmebasi
A, Sorenson EP, et
al. Amyand’s hernia: A review.
Medical Science Monitor 2014.
6. Fouda
JC, Owon’Abessolo PF, Nyanit BD, et al. A case of Amyand hernia at the Central
Hospital of Yaounde and review of the literature. Surg Case Rep 2023;9.
7. Singal R, Gupta S. Maedica-a Journal of Clinical Medicine
“Amyand’s Hernia”-Pathophysiology,
Role of Investigations and Treatment, Maedica J Clin Med 2011.
8. Fezoulidi G, Argyrouli V, Adamopoulos E, et al. Amyand’s hernia: presumptive diagnosis by CT
and literature review. Radiol Case
Rep 2021;16:911-915.