Eagle Syndrome: Two Cases
Abstract
Eagle syndrome is a set of clinical and radiological signs related to calcification of the stylohyoid ligament causing cervicofacial pain.
We report two cases of Eagle syndrome, presenting with cervicofacial pain, provoked by chewing, swallowing and phonation. Clinical examination revealed an indurated mass in the posterolateral floor of the mouth on both sides.
Orthopantomogram and open-mouth head and neck CT scan confirmed the presence of elongation of the styloid process with calcification of the stylohyoid ligaments bilaterally. The treatment of Eagle syndrome is mainly surgical, with clear postoperative progression.
Keywords: Eagle syndrome; Stylohyoid ligament; Cervicofacial pain; Orthopantomogram
The clinical picture is variable and the diagnosis is essentially based on the presence of a cervico-facial pain syndrome, of the migraine type, increasing during chewing, swallowing and head rotation movements, with the presence on imaging of an elongation of the styloid process, accompanied by more or less significant stylohyoid calcification.
The
pain itself is orofacial or cervical, often secondary to tonsillectomy or
wearing an unsuitable dental prosthesis.
Observation and Patient
Case No 1:
This is a
52-year-old patient who consulted for right cervicofacial pain caused by
swallowing, chewing and speaking. This pain has been developing for more than 5
years and has worsened over the past 6 months. The patient has had multiple
dental extractions over the past 6 years, the most recent of which was 1 year
ago.
The clinical
examination showed a patient in good general condition, with a symmetrical face
with a 4cm mouth opening, she is wearing a total dental prosthesis, intraoral
palpation revealed a bony-like protrusion in the bilateral posterolateral oral
floor, in contact with the internal surface of the mandibular angles. Palpation
was painful on the right side and which radiated towards the oral floor, the
homolateral cervical region, then the homolateral hemiface.
The
orthopantomogram (Figure 1) revealed elongation of the styloid process
as well as calcification of the bilateral stylohyoid ligament.
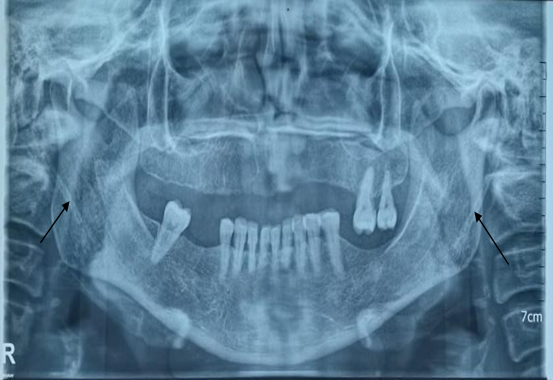
Figure 1: On the panoramic radiograph, the stylohyoid and thyrohyoid ligaments are clearly visible bilaterally, creating a superimposed image relative to the mandibular angle
A cervicofacial CT scan performed with the mouth open (Figure 2) confirms the presence of an elongated styloid process bilaterally with calcification of the stylohyoid ligaments, as well as close relationships existing with the later pharyngeal wall and the floor of the mouth.
Figure 2: On the
3D summation scan image in the open mouth, we note the elongation of the
styloid process as well as its calcified ligament coming in parallel with the
mandibular ascending branch.
The measurements of the right and left styloid processes are 40.9mm and 49.1mm respectively (Figure 3)
Figure 3: 2D summation CT imaging, measurement of the elongation of the two styloid processes
The diagnosis of Eagle syndrome was made and the patient underwent resection of the styloid process on the right side under general anesthesia via a subangular mandibular approach (Figure 4).
Figure 4: The patient underwent a 39mm styloid process resection
Evolution
The symptoms
disappeared immediately post-op, indicating an effective surgical procedure.
No complications
were reported after 3 months and 6 months of follow-up in consultation.
No recurrence of
the symptomatology was expressed by the patient.
Case no 2:
This is a
25-year-old patient who consulted for maxillofacial surgery for bilateral
cervicofacial pain, worse on the right, caused by swallowing, chewing,
phonation and more rarely spontaneous, this pain has been developing for more
than 7 months, the patient reports no surgical history.
The clinical examination found a patient in good general condition, with a symmetrical face with a mouth opening of 3.5 cm, not edentulous, with good dental articulation, intraoral palpation revealed a hardened protrusion in the posterolateral floor of the mouth bilaterally, in contact with the internal face of the mandibular angle on each side, hard and protruding.
Palpation caused pain, identical to that felt by the patient during painful episodes.
The lymph node areas were free.
A cervicofacial CT scan was performed confirming the presence of an elongated styloid process bilaterally with calcification of the stylohyoid ligaments, as well as close relationships existing with the lateropharyngeal wall and the floor of the mouth.
A measurement of the styloid process was carried out on 2D scan imaging (Figure 5) in order to confirm the diagnosis, finding a right process at 34.8mm and a left one at 30.8mm
Figure 5: 2D summation CT imaging, measurement of the elongation of the two styloid processes
The diagnosis of Eagle syndrome was made and the patient underwent resection of the styloid process on the right side under general anesthesia via the subangular mandibular approach (Figure 6).
Figure 6: The patient underwent a resection of the styloid process on the right side with a length of 34 mm
Evolution:
The symptoms
disappeared immediately post-op, indicating an effective surgical procedure.
No complications
were reported after 3 months and 6 months of follow-up in consultation.
No recurrence of
the symptomatology was expressed by the patient.
Discussion
In 1937, Eagle
described pain due to elongation of the styloid process. Ten years later4, he reported 254 cases, 44 of which were
operated on.
Embryologically, the styloid process, the stylohyoid ligament and muscle, the lesser cornua and the upper part of the body of the hyoid bone derive from the 2nd branchial arch, whereas the greater cornua, the lower part of the body and the stylopharyngeus muscle derive from the 3rd branchial arch6. The ossification nuclei are different for each of these structures. Ossification begins in the 5th month of fetal life, so these structures are present at birth.
The styloid process and ossification of the stylohyoid ligament have given rise to various hypotheses. Murtagh, et al7, suggest congenital elongation with persistence of the cartilage matrix cartilage or calcification of the styloid ligament, while Kurmann, et al8, suggest ossification related to aging or mechanical enthesopathy. A histopathological study from the ENT Association of India suggests metaplastic changes due to repetitive or traumatic stress on the stylohyoid ligament and styloid muscles. Some authors note a history of tonsillectomy or surgical trauma10,4,3
Clinically, symptoms usually consist of pharyngeal pain when swallowing or turning the head, associated with muscle spasms.
The pain is typically dull and unilateral. It is located in the oropharynx and may radiate to the ear; it increases with swallowing5. Typically, palpation of the tonsillar cavity reveals a firm to solid element that is very painful to the touch and perfectly reproduces the pain complained of by the patient.
Normally, the styloid process is supposed to measure 25 mm and therefore is not palpable. According to Eagle1,4, the usefulness of radiology was not to establish the surgical indication but above all to estimate the length of bone to be respected, only the clinic allows to establish the surgical indication according to the patient's symptoms.
Nevertheless, many
authors5,8,11,12 have been interested
in the normal length of the styloid process: the average would be around 30 mm,
slightly (1 mm) longer in men and increasing with age to reach 37 mm on average
after 80 years13. More interestingly,
the shape is not always rectilinear but can be angulated or curved in 6-7% and
calcifications along the stylohyoid ligament can be present in 30% of
asymptomatic people.
The assessment of the styloid process is preferably done on CT after injection of contrast agent14,15,16 « fig. 3 » This allows not only to make 2D reconstructions in the axis of the styloid process to precisely measure its length but also to evaluate the thickness of the styloid process as well as the relationship of the styloid process with the neighboring vascular structures, the tonsillar lodge and the constrictors of the pharynx. 3D reconstructions are especially useful to evaluate the spatial relationship between the styloid process and the internal carotid artery « fig.2 ».
The incidence of styloid processes longer than 30 mm remains very variable in the literature, between 0.4% and 84%!17
It is easy to imagine how the styloid process and stylohyoid ligament complex may come into contact with the glossopharyngeal nerve, the carotid vessels or the constrictor muscles of the pharynx. However, a convincing radiological demonstration remains to be demonstrated.
The literature
illustrates two possible therapeutic options: conservative treatment and
surgical treatment
Conservative
treatment is chosen either in the presence of mild or moderate symptoms or if
the patient refuses surgical therapy18.
It is mainly medicinal
In addition to oral medication, analgesic injections through the tonsillar fossa or towards the small horn of the hyoid bone can be performed17Several therapeutic options, including the use of local anesthetics such as lidocaine, steroids such as cortisone or hydrocortisone and impletol (a combination of procaine and caffeine), are available17,19,20. Manual fracture of the styloid process by transpharyngeal manipulation, although suggested as a non-surgical option, has few positive results and carries risks of vascular or nerve damage as well as recurrence21-24. Heat application to painful areas and Chinese medicine are also mentioned in the literature, although their effectiveness remains poorly studied17
Surgery is the
most appropriate treatment for Eagle syndrome. However, it should only be
considered after confirmation of the pathology by radiographic examinations and
after ruling out other head and neck pathologies.
In Eagle's series, all 44 patients were cured3. Even then, the section was done orally, with identification of the bone, dissection and section with scissors or forceps, several procedures have been developed since, but there are only two surgical approaches to treat Eagle syndrome: an intra-oral route and another extra-oral; Two principles must be considered for surgery regardless of the route used, it is important to resect the styloid process as close as possible to its temporal attachment to prevent the risk of recurrence and even if the symptoms are most often unilateral.
Several studies have been carried out comparing the two approaches (trans-oral and trans-cervical)25-28 without significant difference between the two, but reporting the superiority and effectiveness of surgical treatment compared to the conservative procedure
Regarding the transoral approach, it can be performed under local anesthesia or, more frequently, under general anesthesia. If the tonsils are still present, a tonsillectomy is performed. To guide the surgeon, he must palpate the styloid process in the superolateral corner of the tonsillar fossa. He must then incise the mucosa opposite its tip or under the palatoglossal arch by reclining the tensor and levator veli palati. The periosteum of the process is then incised by reclining the muscular and ligamentous attachments towards the temporal bone. The styloid process is then resected as close as possible to its temporal attachment using a rongeur. Finally, the muscles, ligaments and mucosa are sutured in layers. This technique is illustrated in the clinical case presented. Although simple and rapid, this therapy does not leave visible scars. However, the visibility of ts approach is limited, which reduces the control of a correct resection of the styloid process. In addition, access to the surgical site can be difficult in case of limitation of the oral opening29,27,30.
For Toshinori, et
al31, Endoscopic piezoelectric
resection is chosen for a minimally invasive and conservative approach to the
tonsils.
To perform the extraoral surgical approach, a 3 to 4 cm skin incision is made under the mandibular angle following the anterior border of the sternocleidomastoid muscle according to the Sébileau Carrega incision32-34. After identifying the platysma muscle, it and the superficial cervical fascia are resected. This allows the submandibular gland and the anterior border of the sternocleidomastoid muscle to be exposed. The latter is then retracted to allow identification of the stylohyoid muscle, the posterior belly of the digastric muscle and the external carotid artery and its branches. These elements are then retracted to fully expose the styloid process. From this point on, the protocol for this approach is similar to that described previously: the periosteum of the process is incised to allow retraction of its muscular and ligamentous attachments, then the process is resected at its temporal base. Finally, the muscles, ligaments, fascia and mucous membranes are sutured in layers.
In our series, extra-oral transcervical surgery demonstrated its role, the procedure was without complications and the result was relevant for the operator and satisfactory for both patients, with complete disappearance of the discomfort post-operatively.
This cervical
approach to the styloid process is preferred35
because of the better control it offers of the vascular pedicles, possible
better visualization of other cranial nerves and in order to avoid a
pharyngo-cervical fistula[36].
Beyond the cervical scar and possible involvement of the facial nerve branches, exposure towards the base of the skull is far from optimal, for this reason Zheng, et al37, propose intraoperative planning by percutaneous punching, which he describes as not only effective in the treatment of styloid syndrome, but also allows minimally invasive management of the scar first and fewer per- and post-op complications
Conclusion
The clinical
picture of Eagle syndrome is not very specific: it can sometimes lead to
diagnostic errors favored by the lack of knowledge of the pathology and the
multiplicity of differential diagnoses. It is important that this pathology is
known to the practitioner in maxillofacial surgery, who can suspect it from the
history and clinical examination, then confirm it by highlighting a styloid
elongation on a panoramic image.
References
1. Eagle WW. Elongated
Pen Processes: Report of Two Cases. Arch Otolaryngol Head Neck Surg 1937;25(5):584-587.
2. Roseman DM. Carotidynia. A distinct
syndrome. Arch Otolaryngol Chic Ill 1967;85(1):81-84.
3. Dulguerov P, Kohler R, Becker M.
Carotidynia and Eagle syndrome: two classic syndromes to be rediscovered. Rev
Med Suisse 2011;311(35):1929-1934.
4. Eagle WW. Elongated Styloid process;
further observations and a new syndrome. Arch Otolaryngol 1948;47(5):630-640.
5. Thot B, Revel S, Mohandas R, Rao AV, Kumar
A. Eagle’ syndrome. Anatomy of the styloid process. Indian J Dent Res Off Publ
Indian Soc Dent Res 2000;11(2):65‑70.
6. Sadler TW.
Langman’s medical embryology, 7th edition. 7th edition Baltimore: Williams
Wilkins 1995.
7. Murtagh RD, Caracciolo JT, Fernandez G. CT
findings associated with Eagle syndrome. AJNR Am J Neuroradiol 2001;22(7):1401‑1402.
8. Kurmann PT, Van Linthoudt D. Eagle
syndrom: a rare cause of lateral neck pain. Praxis 2007;96(8):297‑300.
9. Jeyaraj P. Histopathological Analysis of
Elongated Styloid Processes: A New Light on Etiopathogenesis of Eagle’s
Syndrome. Indian J Otolaryngol Head Neck Surg Off Publ Assoc Otolaryngol India
2022;74(3):4510‑
4520.
10. Bafaqeeh SA. Eagle syndrome: classic and
carotid artery types. J Otolaryngol 2000;29(2):88‑ 94.
11.
Shibuya
Y, et al. A clinical study of temporomandibular joint disorders -an analysis
based on the Japanese subtype classification. Kobe J Med Sci 2007;53(1‑2):63‑70.
12. Ruddy S, Harris ED,
Sledge CB, Kelley WN. Kelley’s textbook of rheumatology. 6th ed. Philadelphia:
WB Saunders Co 2001.
13. Okabe S, Morimoto Y, Ansai T, et al.
Clinical significance and variation of the advanced calcified stylohyoid
complex detected by panoramic radiographs among 80-year-old subjects. Dento
Maxillo Facial Radiol
2006;35(3):191‑199.
14. Monsour PA, Young WG. Variability of the
styloid process and stylohyoid ligament in panoramic radiographs. Oral Surg
Oral Med Oral Pathol 1986;61(5):522‑526.
15. Ramadan SU, Gokharman D, Tunçbilek I,
Kacar M, Koşar P, Kosar U. Assessment of the stylohoid chain by 3D-CT. Surg
Radiol Anat SRA 2007;29(7):583‑ 588.
16. Singh R, Sharma R, Sharma VK, Prajapati N,
Rana AK. Styloid Process; Correlation Between Symptoms, Palpability and
Measurements on Three-Dimensional Computed Tomography. Indian J Otolaryngol
Head
Neck Surg Off Publ Assoc Otolaryngol India 2022;74(3):5556‑ 5561.
17. Piagkou M, Anagnostopoulou S, Kouladouros
K, Piagkos G. Eagle’s syndrome: a review of the literature. Clin Anat NYN. 2009;22(5):545‑558.
18. Maheshwari S, Panda AK, Rawal M, Singh S,
Madan D. Eagle’s Syndrome with Heterogenic Clinical Manifestation. Neurol India
2022;70(5):2283.
19. Mohanty S, Thirumaran NS, Gopinath M,
Bambha G, Balakrishnan S. Significance of styloidectomy in Eagle’s syndrome: an
analysis. Indian J Otolaryngol Head Neck Surg Off Publ Assoc Otolaryngol India
2009;61(4):262‑265.
20. Balbuena L, Hayes D, Ramirez SG, Johnson
R. Eagle’s syndrome elongated styloid process. South Med J 1997;90(3):331‑334.
21. Masson E. Eagle
syndrome: a poorly understood and poorly recognized pain! EM-Consulte.
22. Khandelwal S, Hada YS and Harsh A. Eagle's
syndrome - A case report and review of the literature. Saudi Dent J 2011;23(4):211-215.
23. Trendel D, Bonfort G, Lapierre-Combes M,
Salf E and Barberot JP. Acute cervical pain and dysphagia after cervical
manipulation: diagnostic approach. Ann Fr Oto-Rhino-Laryngol Pathol
Cervico-Faciale
2014;131(2):121-124.
24. Ceylan A, Köybaşioğlu A, Celenk F, Yilmaz
O, Uslu S. Surgical treatment of elongated styloid process: experience of 61
cases. Skull Base Off J North Am Skull Base Soc Al 2008;18(5):289‑295.
25. Waters CM, Ho S, Luginbuhl A, Curry JM,
Cognetti DM. Surgical Management of Stylohyoid Pain (Eagle’s) Syndrome: A
5-Year Experience. Ann Otol Rhinol Laryngol 2019;128(3):220‑226.
26. Hardin FM, Xiao R, Burkey BB. Surgical
management of patients with Eagle syndrome. Am J Otolaryngol 2018;39(5):481‑484.
27. Wang J, Liu Y, Wang ZB, Yan KS. Intraoral
and extraoral approach for surgical treatment of Eagle’s syndrome: a
retrospective study. Eur Arch Oto-Rhino-Laryngol Off J Eur Fed
Oto-Rhino-Laryngol Soc EUFOS
Affil Ger Soc Oto-Rhino-Laryngol Head Neck Surg 2022;279(3):1481‑1487.
28. Baldino G, Di Girolamo C, De Blasis G,
Gori A. Eagle Syndrome and Internal Carotid Artery Dissection: Description of
Five Cases Treated in Two Italian Institutions and Review of the Literature.
Ann Vasc Surg
2020;67:565.
29. Chrcanovic BR, Custódio ALN, de Oliveira DRF. An intraoral
surgical approach to the styloid process in Eagle’s syndrome. Oral Maxillofac
Surg 2009;13(3):145‑151.
30. Regmi D, Baidhya R, Rajak A, Shrestha S,
Bista M. Trans-oral Extra Tonsillar Approach of Styloidectomy for Treatment of
Eagle’s Syndrome among Operated Cases of the Department of Otolaryngology-Head
and Neck Surgery at a Tertiary Care Hospital: A Descriptive Cross-sectional
Study. JNMA J Nepal Med Assoc 2021;59(240):738‑740.
31. Iwai T, Iida M, Sugiyama S, Mitsudo K.
Intraoral Styloidectomy Using an Endoscope With Tissue Retractor. J Craniofac
Surg 2022;33(4):1201‑1202.
32. Shin JH, Herrera SR, Eboli P, Aydin S,
Eskandar EH, Slavin KV. Entrapment of the glossopharyngeal nerve in patients
with Eagle syndrome: surgical technique and outcomes in a series of 5 patients.
J Neurosurg
2009;111(6):1226‑1230.
33. Papadiochos I, Papadiochou S, Sarivalasis
ES, Goutzanis L, Petsinis V. Treatment of Eagle syndrome with transcervical
approach secondary to a failed intraoral attempt: Surgical technique and
literature review. J
Stomatol Oral Maxillofac Surg 2017;118(6):353‑358.
34. Pigache P, Fontaine C, Ferri J, Raoul G.
Transcervical styloidectomy in Eagle’s syndrome. Eur Ann Otorhinolaryngol Head
Neck Dis 2018;135(6):433‑436.
35. Taneja S, Chand S, Dhar S. Stylalgia and
Styloidectomy: A Review. J Maxillofac Oral Surg 2023;22(1):60‑66.
36. Buono U, Mangone GM, Michelotti A, Longo F,
Califano L. Surgical approach to the stylohyoid process in Eagle’s syndrome. J
Oral Maxillofac Surg Off J Am Assoc Oral Maxillofac Surg 2005;63(5):714‑716.
37. Zheng Y, Yan B, Zhong H, Yi W, Yang Y, Wang
Q. Clinical efficacy of Styloid incision truncation via percutaneous punching
in treating Styloid process syndrome. J Orthop Surg 2023;18(1):38.
38. Choumi F, Ziani Y. Eagle syndrome: a case
report. Pan Afr Med J 2014;18:333.