Enhancing Prescription Practices for Syringe Drivers Among Junior Doctors in Oncology: A Quality Improvement Initiative
Aim
The primary aim of this quality improvement initiative is to evaluate and enhance prescription practices for syringe drivers among junior doctors in the oncology department.
Keywords: syringe drivers; oncology; pharmacist
Introduction
Accurate prescription practices for syringe drivers are essential in oncology care, where errors pose significant risks to patient safety1. An initial assessment identified recurring prescription errors among junior doctors in the oncology department, particularly regarding syringe drivers for patient discharge. These errors not only increase the workload for clinical pharmacists but also introduce potential safety risks. To address these challenges, this quality improvement project was designed to evaluate and improve prescription practices for syringe drivers2.
Methods
A questionnaire assessing knowledge, prescription practices and areas of difficulty related to syringe drivers was administered to 25 doctors, with 23 completing the survey. Following the initial assessment, all resident doctors received comprehensive training that included live demonstration sessions, one-on-one guidance and resources to foster confident and accurate prescribing practices.
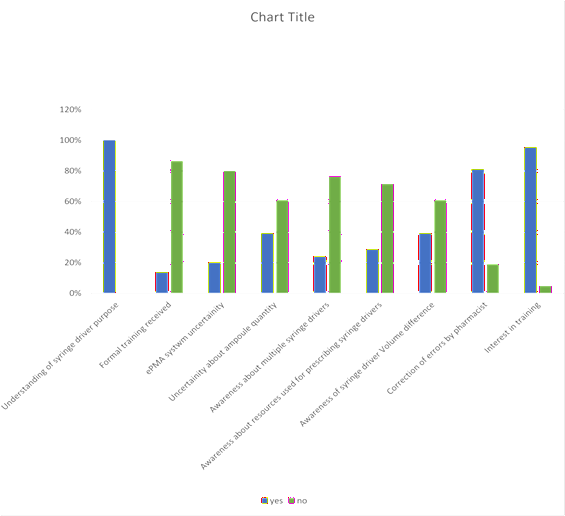
Initial results
• Understanding of syringe driver purpose: 100%
• Formal training received: 13.64%
• Epma system uncertainty: 20%
• Awareness of syringe size differences: 60.87%
• Uncertainty about ampoule quantities: 34.76%
• Belief about single syringe driver: 23.81%
• Correction by pharmacists: 80.95%
• Interest in training: 95.24%
Discussion
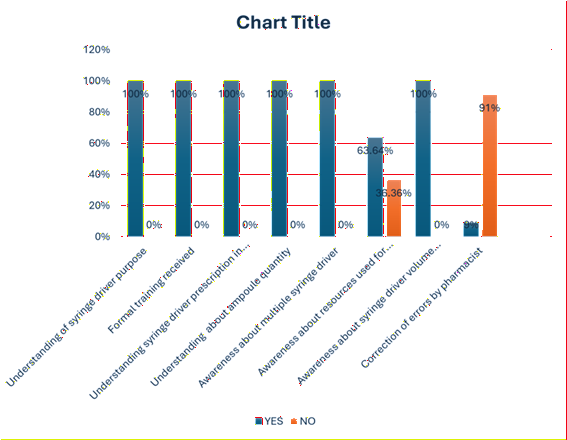
The re-audit results show a significant improvement in
knowledge and prescription practices among junior doctors, indicating that the
targeted interventions effectively addressed prior deficiencies. The reduction
in pharmacist corrections further highlights the impact of the initiative on
improving prescription accuracy and enhancing patient safety.
Conclusion
This project underscores critical areas
for improvement in syringe driver prescription practices among junior doctors.
By implementing targeted training, live demonstration sessions and visual aids,
we have effectively minimized errors and raised awareness of best practices. A
positive departmental change resulting from this project is the new policy of
providing syringe driver demonstration classes to all incoming doctors during
their induction phase, a sustainable measure that promises to maintain high standards
in prescription practices and ensure ongoing patient safety.
References
1. Faull c, windridge k, ockleford e, et al.
Anticipatory prescribing in terminal care at home: what challenges do community
health professionals encounter? Bmj support palliat care 2013;3:91-97.
2. Sheehy-skeffington b, mclean s, bramwell m, et
al. Caregivers experiences of managing medications for palliative care patients
at the end of life: a qualitative study. Am j hosp palliat care 2014;31:148-154.