Mueller-Weiss syndrome: A Radiological Diagnosis
Abstract
Mueller-weiss syndrome is an uncommon condition characterized by the
spontaneous development of osteonecrosis in the navicular bone of adults, with
no known cause. It predominantly affects women, either on one side or both
sides, and can result in significant functional impairment. The diagnosis is
typically made based on clinical observations of mechanical-type pain on the
upper surface of the middle foot and is confirmed through radiological
examinations.
Keywords: mueller-weiss syndrome;
navicular bone; standard x-ray, ct-scan
Introduction
Osteonecrosis of the navicular bone, also
known as muller-weiss syndrome, is a rare condition described in the literature
in 1927 by walther mueller. It occurs in adults between 40 and 60 years of age
and is more frequent in women1. Its varied clinical presentation is
dominated by midfoot and ankle pain. The typical radiological image is a
comma-shaped aspect of the navicular bone2.
The aim of this case is to present the
radiological findings of this disease.
Discussion
First described by
muller and weiss in 1927 yet its pathophysiology is still a matter of debate.
According to some authors, the necrosis may be back up to the mechanical
compression of the navicular bone caused by trauma or increased pressures on
the midfoot arch in flat feet because of being overweight. Others assume that
the unstable vascularization of the navicular bone is the cause of
osteonecrosis1.
Most patients
report experiencing a chronic mechanical pain of gradual onset accompanied by a
deformation of the dorsal part of the midfoot. Their physical examination
recovers tenderness and dorsomedial foot swelling and varus deformity of the
heel.
Standard x-ray is
the first line radiological exploration, including weight bearing
anteroposterior and lateral views, which reveals a characteristic appearance:
- ankle and
hindfoot: the collapse of the lateral half of the navicular bone engenders a
medial subluxation of the talus head which provokes the hindfoot varus (figure 1).
- midfoot: when the
navicular bone’s lateral half falls down, it becomes sclerotic and takes the
aspect of a comma or hourglass (figure 2).
This along with the aforementioned medial subluxation of the talus head,
creates a talo-navicular articulation.
- forefoot: as the
arch of the foot collapses, the metatarsals align in parallele and hypertrophic
changes occur in the second metatarsal due to the force of compression
exercised by the second metatarsal instead of the first one and the
tarsometatarsal articulations.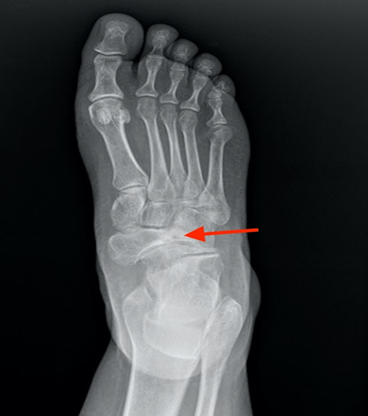
Figure 1. Oblique radiograph of the forefoot showing the
collapse of the lateral part of the navicular bone and the medial subluxation.
(red arrow)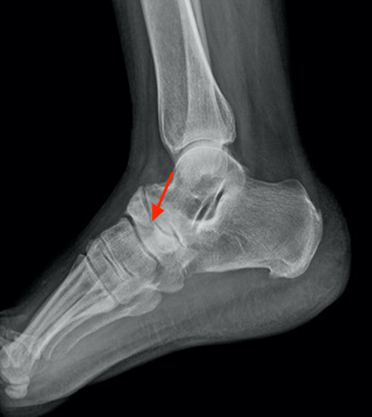
Figure 2. Lateral radiograph of the forefoot revealing a
sclerosis and densification of navicular bone (red arrow).
Maceira and
rochera had also provided a descriptive staging system with 5 degrees of
deformity for the mueller weiss syndrome as assessed on weight bearing lateral
radiographs. The degree of deformity is defined by the navicular bone aspect
and the meary-tomeno angle (the angle formed between the longitudinal axes of
the talus and the first metatarsal). In a normal foot, these axes are aligned.
A meary-tomeno angle superior to 4° convex downwards indicates a flat foot2.
Ct scan is
also useful for diagnosis and plays an important role in the preoperative
assessment by evaluating the bone’s structure and their mineralization (figures 3,4).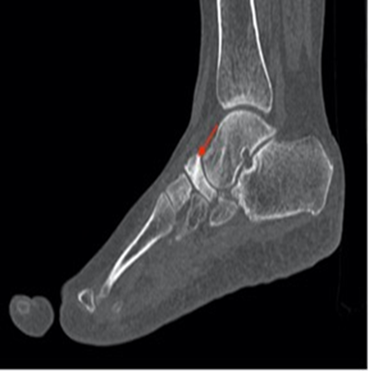
Figure 3. Sagittal ct scan of the forefoot demonstrating the
comma aspect of the navicular bone (red arrow)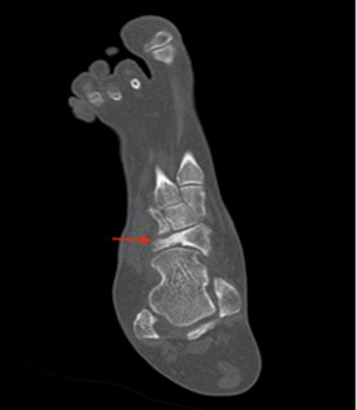
Figure 4. Coronal ct scan illustrating the collapse of the
lateral part of the navicular bone (red arrow) associated with medial
subluxation.
Mri can show oedema on stir / dp fs (short t1 inversion
recovery / density proton with fat saturation) images and is more precise in
detecting early changes because of its ability to detect signal change in the
bone marrow, thereby excluding differential diagnosis as fatigue fracture (overuse
fracture) and infections2,3.
The therapeutic strategy is not unified among authors.
However, the majority of publications advocate for an initial phase of medical
treatment, weight loss, oral anti-inflammatory drugs and immobilization with
orthoses or plaster for a few weeks. The chirurgical treatment depends on the
severity of symptoms and is reserved for cases where medical treatment fails or
for stage 3 and above3.
Conclusion
Mueller-weiss syndrome is a rare,
under-diagnosed and multifactorial condition. It can rapidly lead to
deformities and disability. However, a better understanding of this disease and
its radiological manifestations could allow for earlier diagnosis and better
future management.
Conflicts of interest
This
study does not have any conflict of interest.
References
1. Gargouri m, jallouli m, feki
w, et al. Müller-weiss syndrome: a rare cause of foot pain. Revue med interne
2018;39(suppl.2):172-173.
2. samim m, moukaddam h, smitaman e. Imaging of
mueller-weiss syndrome: a review of clinical presentations and imaging
spectrum. Am j roentgenol. 2016;207(2):8-18.
3. de marchi esn, silveira monteiro s, de avila
fernandes e. Mueller weiss syndrome: case report. Rev ass med bras 2014;60(2):103-104.