Pemphigus Vulgaris
ABSTRACT
Pemphigus is an unusual skin disease characterized by
blistering of the skin and mucous membranes.
It has a predilection
for people of middle or advanced age; clinically it manifests with the
appearance of blisters in the oral and genital mucosa, face, and extremities
which are usually painful but do not cause itching. It can reach a mortality of
up to 75% without treatment.
Keywords:
Pemphigus vulgaris; Blister; Desmoglein
Abbreviations:
DSG 3: Desmoglein 3
IL4: Interleukin 4
DSG1: Desmoglein 1
INTRODUCTION
Pemphigus, a term from Greek meaning blister, is a rare,
chronic, autoimmune vesiculobullous disease that attacks the mucous membranes
and skin. There are two main types; pemphigus vulgaris and
foliaceous. Other classifications of pemphigus include paraneoplastic,
erythematous, vegetative, and IgA subtypes. The diagnosis depends on clinical
suspicion and confirmation by biopsy which demonstrates intraepithelial vesicle
formation, acantholysis1. A Tzanck
test which can be performed bedside demonstrates the presence of acantholytic
cells.
In pemphigus vulgaris there are autoantibodies directed
against Dsg1, mainly located in the superficial layers of the epidermis and Dsg
3, which tends to the basal layers. The formation of these autoantibodies is
associated with the presence of CD4+ Th2 lymphocytes, which mainly secrete IL-42; this induces a humoral immune response that
promotes the differentiation of B lymphocytes into IgG4-secreting cells present
in patients with pemphigus vulgaris and pemphigus foliaceus.
CASE PRESENTATION
A
36-year-old female patient, with history of left ovarian cancer, gastritis,
duodenitis and hypothyroidism presented tense, painful blisters beginning in the oral mucosa which generalized to
the upper limbs, then chest, then full body surface over the course of 3 months
(Figure 1 and Figur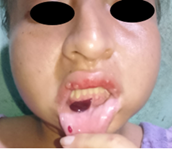
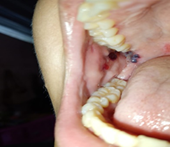
Figure 1. Dermatosis
located at the level of the oral mucosa characterized by blisters, with
serohematic content.
She
was treated in a primary care unit where she received treatment with prednisone
60 mg/day. As her conditioned worsened, she was admitted to Hospital Eugenio
Espejo, a tertiary care center, in Quito. She presented tense blisters at the
level of the left upper limb and multiple post-inflammatory spots, as well as
gastroesophageal reflux. At the time of admission, she had been without
treatment for one month, so intravenous methylprednisolone at 1gram daily for
three doses was instituted, resulting in a significant remission (Figure 3).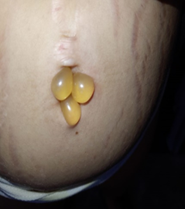
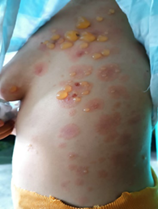
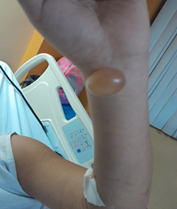
Figure
2. Dermatosis
located at the level of the left rib cage, periumbilical area and left forearm
characterized by tense blisters with serous content, on an erythematous base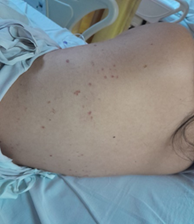
Figure 3. Post-inflammatory spots.
DISCUSSION
Pemphigus vulgaris is a rare chronic blistering disease mediated by antibodies
against adhesion molecules on keratinocyte cell surface. Factors such as
increased age, comorbidities and larger affected body surface define the
evolution and prognosis of the pathology3.
The
prevalence is 0.5 to 3.2 cases per 100,000 inhabitants and the incidence is 0.1
to 0.5 per 1000,000 inhabitants. Clinically, 75% of pemphigus vulgaris begin in
the oral mucosa, initially being small blistering lesions that break easily,
causing painful and bleeding erosions.
In
the majority of patients, the cutaneous phase begins three months after the
appearance of lesions in the oral mucosa. On the skin they appear in the same
way as on the mucous membranes, on normal or slightly erythematous skin,
located anywhere on the body, most frequently on the face, trunk and scalp. The
diagnosis is made based on clinical suspicion and confirmed with biopsy4.
Thanks
to the introduction of corticosteroid therapy, mortality has decreased, the
main cause of mortality being associated with infections and hydroelectrolyte
imbalance.
CONCLUSIONS
Although
it is a rare, autoimmune, rare and chronic disease, early diagnosis is
important since its outcome can be fatal. Early diagnosis occurs through the
detection of lesions in the oral mucosa, since the majority of cases begin at
this anatomical site, relating and evaluating the accompanying comorbidities
and the level of extension in order to provide adequate management.
Conflict of
Interest: The authors declare no conflicts of
interest.
References
Vanessa GR
Cecilia Fanny CM, Judith DC, Silvia MF. Pemphigus vulgaris. Internal
Med Max 2019;35(5): 708-712.
2.
Leiva EV, Kellendok JB, Kellendok AM, Portilla W.
Pénfigo Vulgar, reporte de un caso clínico. CAMbios-HECAM 2019;14(24):78-81.
3. López IBH, Tarragó JM, Pénfigo Vulgar. Criterios Actuales, Rev haban cienc méd 2009;8(5).
4. Sánchez-Pérez J, García-Díez A, Pénfigo, Servicio de Dermatología. Hospital
Universitario de La Princesa 2005;329-356.