Zoon´s Vulvitis: A Rare Differential Diagnosis of Vulvar Pruritus
Keywords: Zoon vulvitis; Plasma cells; Pruritus; Vulva
1. Introduction and contextualization
Zoon´s
vulvitis, also known as plasma cell vulvitis (PCV) is an inflammatory disorder
of the female genital tract, which was first described by Zoon in the 1950s.
Its true etiopathogenesis is unknown, although a variety of triggering factors
have been hypothesized (autoimmune, irritative, hormonal). It typically affects
the vulva, but there are also several case reports of vagina and cervix´s
involvement by this condition1-5. Its real
prevalence is not known, but it´s supposed to be underreported as its typical
symptoms can mimic and be misdiagnosed as other more common vulvovaginal
disorders, such as lichen sclerosus, lichen planus, genitourinary syndrome of
menopause, contact dermatitis or infectious vaginitis6-11.
It
usually presents as a well-circumscribed and erythematous patch/macule with a
fainted red-orange hue involving the vulvar vestibule, periurethral area and
labia minora and majora; it can cause itching, burning, dysuria and
dyspareunia. When the vagina is affected, it can trigger a yellow
leukorrhea-type discharge. Some patients can also be completely asymptomatic.
Histologically, it is characterized by a thinned epithelium with infiltration
of more than 50% of polyclonal plasma cells in the underlying dermis along with
diamond shaped keratinocytes and extravasation or hemosiderin deposition1-4,6,12,13.
The
condition is often difficult to treat, and standard treatment has not been
established9,10. It may include
topical, oral, intralesional and surgical options in refractory cases.
2. Materials & Methods
We
present a case of Zoon´s vulvitis which was treated with corticosteroid therapy
resulting in symptom relief.
3. Results
& Discussion
A
73-year-old patient was referred to a gynecology consultation due to complaints
of persistent vulvar itching and discomfort for the past 6 months. The patient
referred dyspareunia and burning but denied any vaginal discharge. When
symptoms first began, she was evaluated by her primary care provider, who
prescribed topical antifungal, a course of corticosteroid therapy (clobetasol
0.05% ointment) along with an antihistamine (25mg hydroxyzine pills). She was
also recommended to wear looser-fitting clothing. However, despite a partial
initial improvement, itching persisted, and it got worse over time.
The
patient had a personal history of hypertension and dyslipidemia and was taking
medication for both. She has had a hysterectomy with bilateral
salpingo-oophorectomy at 49 years old because of abnormal uterine bleeding
conditioned by uterine leiomyomas. The patient had no known drug allergies.
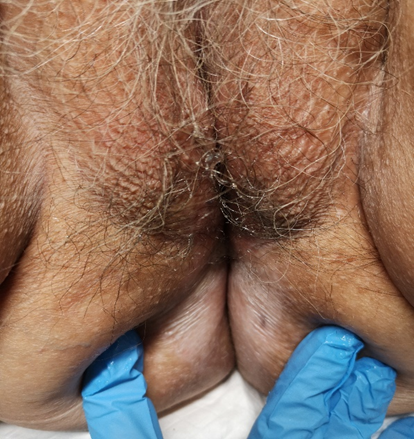
On
examination, the patient presented marked vulvovaginal atrophy, with a whitish
color along both labia minora, inner half of the labia majora and extending to
the perianal region. In the anterior one-third of the transition between the
left labia minora and the labia majora, the presence of a 4mm ecchymotic macule
was notable, and this location corresponded to the area in which the patient
reported the greatest intensity of complaints. There was a similar, but smaller
lesion on the right side (Figure 1).
Figures 1. Clinical aspect of the
patient´s vulva; the circle delimits the area that was initially biopsied.
At
this time, another course of corticosteroid therapy was attempted, and the
patient began topical estrogen therapy. Testing for bacterial vaginosis and the
most common sexual transmitted diseases [trichomonas, chlamydia, gonorrhea,
human immunodeficiency virus (HIV), syphilis, and hepatitis] were also done.
The results were all negative.
She
came back eight weeks later, and the same complaints persisted. The lesion
previously described remained like the first description. In this sense, it was
decided to carry out a punch biopsy at this specific location. A 9mm length
cylindrical punch was obtained, which showed plasmacytosis mucosae consistent
with Zoon´s vulvitis.
The
patient remains under follow-up at a gynecology consultation, complaining of
occasional itching. She maintains topical estrogen therapy and regimens of
topical corticosteroids when the condition worsens.
Vulvovaginal
erythema and/or pruritus may be caused by a range of conditions that varies
from infectious, immunological, or even malignant causes6,7.
Our
patient was older than the average age of patients reported to have this
condition (between 52 and 55 years old)14-16. This fact,
together with the greater probability of other conditions in this age group,
may have contributed to some delay in diagnosis.
As
performed in this case, patients with severe and unresponsive symptoms should
undergo tissue diagnosis to guide the most appropriate treatment. A plasma cell
inflammatory infiltrate is the most common finding on histopathology, which was
consistent with our results.
As
described by Krapf et al.´s review, the most common treatment modalities for
this disorder includes topical corticosteroids and immunomodulation with
tacrolimus and imiquimod, with 88% of patients achieving symptom resolution16.
4. Conclusion
This
case demonstrates the importance of performing a biopsy in timely diagnosis and
treatment, as missed diagnosis can result in delays in instituting therapy and
potential long-term complications.
It is
advised that patients have regular clinical follow-up as periods of remission
and relapse are frequent; although there are no reports of malignant changes of
Zoon´s vulvitis cases, moderate dysplasia has been described17,18.
Although
rare, this condition can cause serious discomfort to patients; therefore, more
research is needed to establish its most cost-effective management.
Acknowledgements
The
authors declare that they have no conflict of interest regarding the
publication of this case report.
No
funding from an external source supported the publication of this case report.
Fernanda
Alves contributed to the conception of the case report, acquiring the data and
undertaking the literature review and drafting the manuscript.
Both
Mara Rocha and Ana Moreira contributed to drafting the manuscript and
undertaking the literature review.
All
authors contributed to revision of the manuscript and approved the final
submitted version.
References
5.
Zoon JJ. Benign chronic
circumscribed balanoposthitis with plasma cells. Dermatologica. 1952;105:1-7.
6.
Simonetta C, Burns
EK, Guo MA. Vulvar dermatoses: a review and update. Mo Med 2015;112:301-307.
17. Joshi VY. Carcinoma of the
penis preceded by Zoon´s balanitis. Int J STD AIDS 1999;10(12):823-825.
18. Vilmer C, Cavelier-Balloy B,
Brousse C, Civatte J. Vulvate plasma cell vulvitis Zoon's benign circumscribed
erythmatous erythroplastic type. Rev Eur Dermatol MST 1990;2:87 94.