Comparative Study of Fine Needle Aspiration Cytology and Histopathology Results of Salivary Gland Swelling in St. Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia
Abstract
Background:
Fine-Needle Aspiration Cytology (FNAC) is a widely accepted, safe, and
cost-effective diagnostic tool for evaluating salivary gland swellings. It
helps differentiate between benign, inflammatory, and malignant lesions, aiding
in surgical planning and management.
Objective:
This study aimed to compare FNAC results with histopathology findings to assess
the diagnostic accuracy of FNAC in evaluating salivary gland swellings at St.
Paul’s Hospital Millennium Medical College, Addis Ababa, Ethiopia.
Methods:
A four-year hospital-based cross-sectional study was conducted on patients with
salivary gland swellings who underwent both FNAC and histopathology at St.
Paul’s Hospital Millennium Medical College from January 1, 2019, to August 30,
2022. Data were collected using a standardized questionnaire and analyzed using
SPSS version 27. Sensitivity, specificity, Positive Predictive Value (PPV), Negative
Predictive Value (NPV), and accuracy were calculated using histopathology as
the gold standard.
Results:
Of the 475 FNACs performed, 110 cases had correlating histopathology results.
The parotid gland was the most commonly affected site (46.4%), followed by the
submandibular gland (42.7%) and minor salivary glands (10.9%). FNAC
demonstrated high sensitivity, specificity, and accuracy: 100%, 98.83%, and
99.09% for non-neoplastic lesions; 96.4%, 92.6%, and 94.5% for benign
neoplasms; and 83.3%, 95.5%, and 94.54% for malignant neoplasms, respectively.
Conclusion: FNAC is a highly sensitive and specific diagnostic tool for evaluating salivary gland swellings. It is reliable for preoperative planning and can help avoid unnecessary surgical interventions.
Keywords: Salivary gland, Fine needle aspiration cytology, Histopathology, Diagnostic accuracy
1.
Introduction
1.1.
Background of the study
Salivary
gland swellings can result from tumors, inflammatory processes, or cysts.
Salivary gland tumors account for approximately 3% of all head and neck
malignancies, with the majority of these neoplasms being benign1,2. Malignant salivary gland tumors represent
only 20% of cases, and the annual incidence of salivary gland cancers is
reported to be 0.5 to 2 per 100,000 people. These tumors affect both men and
women equally, with the majority of cases occurring in the sixth decade of life3. Tumors can develop in both the major and
minor salivary glands, with the parotid glands accounting for 80% of major
salivary gland tumors, while the palate is the most common site for minor
salivary gland tumors4.
Clinical
practice has shown that the smaller the salivary gland, the more likely the
tumor is malignant. Around 20% to 25% of tumors in the parotid glands are
malignant, while this percentage increases to 40% in the submandibular glands,
and over 90% of sublingual gland tumors are malignant3,5. The parotid gland accounts for 75% of
salivary gland tumors, while the submandibular glands contribute 25%. Minor
salivary glands and the sublingual glands account for 8% and 1%, respectively.
The most common benign tumor is pleomorphic adenoma, which is predominantly of
parotid gland origin. Among malignant tumors, mucoepidermoid carcinoma is the
most common, while adenoid cystic carcinoma is the most common malignant tumor
in the submandibular and minor salivary glands6.
Non-neoplastic
lesions of the salivary glands are often caused by chronic sialadenitis,
followed by retention cysts. Salivary gland cystic abnormalities can be
classified as either true cysts (e.g., lymphoepithelial cysts) or
non-developmental cysts (e.g., retention cysts)7,8.
Fine
Needle Aspiration Cytology (FNAC) has proven to be an efficient, simple, and
safe method for evaluating salivary gland enlargement. FNAC boasts high
sensitivity, specificity, and accuracy in identifying salivary gland lesions1,2. The sensitivity of FNAC for salivary gland
lesions ranges from 86% to 100%, while specificity ranges from 90% to 100%8. The accuracy of FNAC is highly dependent on
the experience of both the pathologist and the clinician performing the
aspiration1. FNAC is crucial in treatment
planning, as it allows clinicians to avoid unnecessary surgeries and reduces
healthcare costs9. While open biopsy
may provide diagnostic information, it is generally avoided due to its
invasiveness, which can complicate subsequent surgical interventions10.
1.2.
Statement of the problem
Salivary
gland swellings represent a diverse and challenging group of disorders with
variable clinical presentations, making accurate diagnosis essential1. While Fine-Needle Aspiration Cytology (FNAC)
is widely used for the preoperative evaluation of head and neck tumors, its
accuracy in diagnosing salivary gland masses remains debated in comparison to
other diagnostic modalities. FNAC is a commonly performed, safe, and typically
well-tolerated procedure that provides valuable diagnostic information. The
primary goal of FNAC in salivary gland swelling is to distinguish between
inflammatory and reactive processes, identify benign versus malignant
neoplasms, and provide a definitive diagnosis when possible.
The
accuracy of FNAC significantly impacts the surgical management of salivary
gland swellings. It has been suggested that preoperative FNAC results play a
key role in determining the management strategy for salivary gland swellings,
including the decision to proceed with surgery. Knowing whether a lesion is
malignant or benign in advance can help clinicians tailor surgical approaches,
which could potentially delay or expedite intervention. Despite the unknown
prevalence of salivary gland swellings in our region, many patients with these
swellings present to our institution for diagnosis and management. Given the
limited access to advanced imaging modalities such as CT or MRI, clinicians
rely heavily on FNAC and clinical examination to guide their decisions. This study
aims to correlate FNAC diagnoses with histopathology and assess the sensitivity
and specificity of FNAC in diagnosing salivary gland swellings in our
institution.
1.3.
General objective
The general objective of this study is to compare the FNAC results with histopathology findings of salivary gland swellings in order to assess its diagnostic accuracy among patients who had both FNAC and histopathology results at Saint Paul’s Hospital Millennium Medical College, Department of ORL HNS, and the Oral and Maxillofacial Surgery Department in Addis Ababa, Ethiopia, from January 1, 2019, to August 30, 2022, G.C.
1.4.
Specific objectives
The specific objectives of this study are as follows:
To determine the
accuracy of FNAC diagnosis of salivary gland swelling when compared with
histopathology.
To evaluate the
sensitivity and specificity of FNAC in diagnosing salivary gland swellings in
our institution.
To identify the
patterns of etiology of salivary gland swellings in our institution.
1.5. Significance of the study
The surgical management of salivary gland swellings is increasingly dependent on preoperative FNAC results. This study aims to evaluate the sensitivity, specificity, positive predictive value, negative predictive value, and accuracy of FNAC in diagnosing salivary gland swellings in our institution. These diagnostic metrics will help guide surgeons in determining how much reliance should be placed on FNAC findings in their preoperative decision-making process. By improving the accuracy of preoperative diagnoses, this study may contribute to more informed surgical decisions, optimizing patient outcomes, and potentially reducing unnecessary surgeries.
2.
Methods
2.1.
Study setting and period
The
study was conducted at Saint Paul’s Hospital Millennium Medical College in
Addis Ababa, Ethiopia, over the period from January 1, 2019, to August 30,
2022, G.C. Data collection took place from September 1-8, 2022, G.C.
2.2.
Study design
This
was a hospital-based cross-sectional study conducted on patients admitted to
Saint Paul’s Hospital Millennium Medical College, within the Department of ORL
HNS and the Oral and Maxillofacial Surgery Department, who presented with
salivary gland swelling between January 1, 2019, and August 30, 2022, G.C. The
study involved comparing FNAC results to histopathology reports for salivary
gland swellings. We assessed the diagnostic accuracy of FNAC by calculating its
sensitivity, specificity, positive predictive value (PPV), negative predictive
value (NPV), and overall accuracy in comparison to histopathology results.
2.3.
Study population
The
source population included all patients with salivary gland swellings admitted
to Saint Paul’s Hospital Millennium Medical College, Department of ORL HNS, and
the Oral and Maxillofacial Surgery Department from January 1, 2019, to August
30, 2022, G.C. The study population comprised patients who had both FNAC and
histopathology results and were diagnosed with salivary gland tumors, cysts, or
inflammation during the study period.
2.4.
Eligibility criteria
2.4.1.
Inclusion criteria: All patients with salivary gland swellings
who had both FNAC and histopathology results during the study period.
2.4.2. Exclusion criteria: Patients without FNAC or histopathology results were excluded from the study. Patients with acute infections (viral or bacterial causes) were also excluded from the study.
2.5.
Sample size determination
The sample size was calculated using a single population proportion formula, based on a 7% prevalence of salivary gland swellings from a prior study conducted at Addis Ababa University. The formula used was:
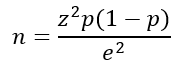
n
= the required sample size
p
= proportion of patients who have salivary gland swelling.
Zα\2
= the critical value at 95% confidence level = 1.96
e
= precision (margin of error) = 5%
Accordingly,
Adding a non-response rate of 10% the final sample size will be 110.
2.6.
Sampling procedure
A
non-probability convenience sampling method was used to select patients from
the study population.
2.7. Study variables
Benign
salivary tumors: Pleomorphic adenoma, Warthin’s tumor,
Basal cell adenoma, Myoepithelioma, Hemangioma, Lymphoepithelial lesions.
Malignant
salivary tumors: Mucoepidermoid carcinoma, Adenoid cystic
carcinoma, Adenocarcinoma, Ex-pleomorphic carcinoma, Acinar cell carcinoma,
Myoepithelial carcinoma, Basal cell carcinoma, Papillary cystadenocarcinoma.
Non-neoplastic
salivary tumors: Chronic sialadenitis, Vascular lesion,
Unspecified cyst, Mucocele.
2.7.2. Independent variables:
Sociodemographic variables: Age, sex, side of swelling (left, right, bilateral), duration of swelling, and affected gland (parotid, submandibular, sublingual, minor salivary gland).
2.8. Operational definitions
Fine
Needle Aspiration Cytology (FNAC): A diagnostic procedure where
a thin needle is inserted into a salivary gland mass to aspirate cells, which
are then examined microscopically.
Histopathology:
The study of tissues for diagnosing diseases, involving microscopic examination
of tissue biopsies, which serves as the gold standard diagnostic method.
Benign
tumors: Tumors that resemble the tissue of origin, lack
invasion, and exhibit mild growth with normal mitotic figures.
Malignant
tumors: Tumors that are poorly differentiated, show a high
mitotic rate, and have invasive and metastatic potential.
Chronic
sialadenitis: Chronic inflammation of the salivary
glands characterized by macrophages, monocytes, lymphocytes, and proliferating
blood vessels and connective tissue.
Mucocele: A cystic swelling caused by disruption of normal salivary secretion flow.
2.9. Data collection procedures and tools
The
data were collected through a review of patient medical records, using
well-standardized and pre-tested questionnaires. The data collection was
conducted by trained ORL HNS residents.
2.9.1.
Data quality assurance: To ensure the accuracy of the data,
a well-trained data collector and supervisor were assigned to monitor data
collection. All collected data were reviewed and checked daily for
completeness.
2.10.
Data analysis procedure
The
collected data were verified for completeness before entering the analysis
phase. Incomplete or erroneous data were cleaned and removed. The final dataset
was entered into SPSS version 27 for analysis. Descriptive statistics,
including tables, charts, and graphs, were used to present the
socio-demographic characteristics of the study population. The diagnostic
accuracy of FNAC was assessed by calculating its sensitivity, specificity,
positive predictive value, negative predictive value, and overall accuracy in
comparison to histopathology.
2.11.
Dissemination of results
Upon completion of the study, the results will be submitted to the relevant departments at Saint Paul’s Hospital Millennium Medical College, including the ORL HNS, Oral and Maxillofacial Surgery, and Pathology Departments. Additionally, the findings will be prepared for publication in peer-reviewed scientific journals and presented at relevant scientific conferences to ensure broader dissemination of the results.
3. Results
3.1.
Socio-demographic characteristics of study participants
A
total of 110 patients were included in the study, with 60 females (54.5%) and
50 males (45.5%). The female-to-male ratio was approximately 1.2:1. The mean
age of the participants was 37.5 ± 16.9 years,
with an age range of 12 to 79 years (Table 1).
Table 1: Socio-demographic characteristics of patients with salivary gland swelling and operated at SPHMMC, Addis Ababa Ethiopia, 2022.
|
Variables |
Frequency (%) |
|
Age Group |
|
|
20-Nov |
16(14.5) |
|
21-29 |
24(21.8) |
|
31-39 |
24(21.8) |
|
41-49 |
18(16.4) |
|
51-59 |
17(15.5) |
|
61-69 |
8(7.3) |
|
71-79 |
3(2.7) |
|
Gender |
|
|
Male |
50(45.5) |
|
Female |
60(54.5) |
The
average duration of salivary gland swelling was 2.95 years, with a minimum
duration of 5 months and a maximum of 15 years. Regarding the laterality of the
swelling, 60 (54.5%) of the cases presented with left-sided swelling, while 50
(45.5%) presented with right-sided swelling.
Regarding the distribution of salivary gland swellings, the parotid gland was most frequently involved (46.4%), followed by the submandibular gland (42.7%), minor salivary glands (10.9%), and the sublingual gland (0%) (Table 2, Figure 1).
Table 2: Site of salivary gland swelling with histopathology results at SPHMMC, Addis Ababa Ethiopia, 2022.
|
Site of swelling |
Frequency (%) |
|
Minor salivary gland |
12(10.9) |
|
Parotid |
51(46.4) |
|
Submandibular |
47(42.7) |
|
Total |
110 |
Figure 1: Site of salivary gland swelling with histopathology results at SPHMMC, Addis Ababa Ethiopia, 2022.
Among the parotid gland swellings, 54.9% were benign lesions, with pleomorphic adenoma (43.1%) being the most prevalent benign lesion. Non-neoplastic lesions, primarily chronic sialadenitis, accounted for 46.8% of submandibular swellings. Mucoepidermoid carcinoma was the most frequent malignant histopathological finding in the parotid, submandibular, and minor salivary glands (Figures 2,3 and 4).
Figure 2: Site of salivary gland swelling with histopathology malignant result at SPHMMC, Addis Ababa Ethiopia, 2022.
Figure 3: Site of salivary gland swelling with histopathology benign result at SPHMMC, Addis Ababa Ethiopia, 2022.
Figure 4: Site of salivary gland swelling with histopathology non neoplastic result at SPHMMC, Addis Ababa Ethiopia, 2022.
3.2. FNAC results
FNAC
results revealed that 27 cases (24.5%) were diagnosed as malignant, 58 cases
(52.7%) as benign tumors, and 25 cases (22.7%) as non-neoplastic lesions.
Pleomorphic adenoma was the most common benign tumor, accounting for 52 cases
(89.65%), followed by lymphoepithelial lesions (3 cases, 5.1%), basal adenoma
(2 cases, 3.4%), and hemangioma (1 case, 1.7%).
Among
the malignant tumors diagnosed by FNAC, mucoepidermoid carcinoma was the most
frequently observed, accounting for 14 cases (51.85%). Other malignant tumors
included adenoid cystic carcinoma (4 cases, 14.81%), undifferentiated carcinoma
(2 cases, 7.4%), ex-pleomorphic adenocarcinoma (2 cases, 7.4%), acinic cell
carcinoma (2 cases, 7.4%), carcinosarcoma (1 case, 3.7%), ductal carcinoma (1
case, 3.7%), and adenocarcinoma (1 case, 3.7%).
Among
the non-neoplastic lesions, chronic sialadenitis was the most common (21 cases,
84%), followed by unspecified cyst lesions (3 cases, 12%) and mucocele (1 case,
4%) (Table 3).
Table 3: FNAC result and its cytology subtype of lesion of salivary gland swelling at SPHMMC, Addis Ababa Ethiopia, 2022.
|
Variables |
Frequency(%) |
|
FNAC result |
|
|
Benign |
58(52.7) |
|
Malignant |
27(24.5) |
|
Non neoplastic |
25(22.7) |
|
Total |
110 |
|
Sub type of Benign
lesion |
|
|
Basal adenoma |
2(34.4) |
|
Hemangioma |
1(1.72) |
|
Lymphoepithelial lesion |
3(5.1) |
|
Pleomorphic adenoma |
52(89.65) |
|
Total |
58 |
|
Sub type of Malignant
lesion |
|
|
Acinic cell carcinoma |
2(7.4) |
|
Adenocarcinoma |
1(3.7) |
|
Adenoid cystic carcinoma |
4(14.8) |
|
Carcinosarcoma |
1(3.7) |
|
Ductal carcinoma |
1(3.7) |
|
Ex pleomorphic adenoma |
2(7.4) |
|
Mucoepidermoid carcinoma |
14(51.85) |
|
Undifferentiated
carcinoma |
2(7.4) |
|
Total |
27 |
|
Non neoplastic sub type |
|
|
Chronic sialadenitis |
21(84) |
|
Mucocele |
1(4) |
|
Unspecified cystic
lesion |
3(12) |
|
Total |
25 |
3.3.
Histopathology results
The
final histopathologic diagnosis revealed 30 malignant tumors (27.3%), 56 benign
tumors (50.9%), and 24 non-neoplastic lesions (21.8%).
The
most common malignant tumor was mucoepidermoid carcinoma, observed in 17 cases
(56.66%), followed by adenoid cystic carcinoma (3 cases, 10%), ductal carcinoma
(2 cases, 6.66%), acinic cell carcinoma (2 cases, 6.66%), ex-pleomorphic
adenocarcinoma (2 cases, 6.66%), myoepithelial carcinoma (2 cases, 6.66%),
adenocarcinoma (1 case, 3.33%), and carcinosarcoma (1 case, 3.33%).
Among
the benign lesions, pleomorphic adenoma was the most prevalent, seen in 48
cases (85.7%), followed by basal adenoma (4 cases, 7.1%), lymphoepithelial
lesions (3 cases, 5.3%), and hemangioma (1 case, 1.7%).
Chronic
sialadenitis was the most common non-neoplastic lesion, accounting for 20 cases
(83.3%), followed by unspecified cyst lesions (3 cases, 8.33%) and mucocele (1
case, 4.16%) (Table 4).
Table 4: Histopathology result and its subtype of lesion of salivary gland swelling and operated at SPHMMC, Addis Ababa Ethiopia, 2022.
|
Variables |
Frequency(%) |
|
Histopathology
result |
|
|
Benign |
56(50.9) |
|
Malignant |
30(27.3) |
|
Non neoplastic |
24(21.8) |
|
Total |
110 |
|
Malignant subtype |
|
|
Acinic cell carcinoma |
2(6.66) |
|
Adenocarcinoma |
1(3.33) |
|
Adenoid cystic carcinoma |
3(10) |
|
Carcinosarcoma |
1(3.33) |
|
Ductal carcinoma |
2(6.66) |
|
Ex pleomorphic adenoma |
2(6.66) |
|
Mucoepidermoid carcinoma |
17(56.66) |
|
Undifferentiated carcinoma |
2(6.66) |
|
Total |
30 |
|
Benign subtype |
|
|
Basal adenoma |
4(7.1) |
|
Hemangioma |
1(1.7) |
|
Lymphoepithelial lesion |
3(5.3) |
|
Pleomorphic adenoma |
48(85.7) |
|
Total |
56 |
|
Non neoplastic subtype |
|
|
Chronic sialadenitis |
20(83.33) |
|
Mucocele |
1(4.16) |
|
Unspecified cystic lesion |
39(12.5) |
|
Total |
24 |
3.4.
Discordant results between FNAC and histopathology
Discordant results were observed in 16 cases, where the FNAC diagnosis did not match the histopathology findings. Specific discordances included:
One case of
carcinoma ex-pleomorphic adenoma, which was diagnosed as pleomorphic adenoma by
FNAC.
Three cases
diagnosed as mucoepidermoid carcinoma on histopathology were diagnosed as
pleomorphic adenoma by FNAC.
One case of acinic
cell carcinoma was misdiagnosed as ductal cell carcinoma by FNAC.
Two cases of
ductal cell carcinoma were diagnosed as undifferentiated carcinoma and acinic
cell carcinoma by FNAC.
Two cases of
myoepithelial carcinoma were diagnosed as mucoepidermoid carcinoma and adenoid
cystic carcinoma by FNAC.
Two cases of basal
adenoma were diagnosed as pleomorphic adenoma by FNAC.
Two cases of
pleomorphic adenomas were diagnosed as mucoepidermoid carcinoma by FNAC.
Three cases of mucoepidermoid carcinoma were diagnosed as chronic sialadenitis, ex-pleomorphic adenoma, and undifferentiated carcinoma by FNAC (Table 5).
Table 5: Cases with discordant in cyto histopathological diagnosis, SPHMMC, Addis Ababa, Ethiopia,2022.
|
Cytology diagnosis |
Histopathology diagnosis |
|
Pleomorphic adenoma |
Basal adenoma |
|
Pleomorphic adenoma |
Basal adenoma |
|
Pleomorphic adenoma |
Mucoepidermoid carcinoma |
|
Pleomorphic adenoma |
Mucoepidermoid carcinoma |
|
Pleomorphic adenoma |
Mucoepidermoid carcinoma |
|
Pleomorphic adenoma |
Ex pleomorphic adenoma |
|
Chronic sialadenitis |
Mucoepidermoid carcinoma |
|
Ductal carcinoma |
Acinic cell carcinoma |
|
Ex pleomorphic adenoma |
Mucoepidermoid carcinoma |
|
Mucoepidermoid carcinoma |
Myoepithelial carcinoma |
|
Acinic cell carcinoma |
Ductal carcinoma |
|
Mucoepidermoid carcinoma |
Pleomorphic adenoma |
|
Mucoepidermoid carcinoma |
Pleomorphic adenoma |
|
Undifferentiated carcinoma |
Ductal carcinoma |
|
Undifferentiated carcinoma |
Mucoepidermoid carcinoma |
|
Acinic cell carcinoma |
Myoepithelial carcinoma |
3.5. Diagnostic accuracy assessment
The
diagnostic accuracy of FNAC was evaluated by calculating its sensitivity,
specificity, Positive Predictive Value (PPV), Negative Predictive Value (NPV),
and overall accuracy for each category of salivary gland pathology.
· Benign cases:
o
Sensitivity: 96.42%
o
Specificity: 92.6%
o
Positive Predictive Value (PPV): 93.1%
o
Negative Predictive Value (NPV): 96.1%
o
Accuracy: 94.54%
·
Malignant cases:
o
Sensitivity: 83.3%
o
Specificity: 95.5%
o
PPV: 92.6%
o
NPV: 93.97%
o
Accuracy: 93.63%
·
Non-neoplastic cases:
o
Sensitivity: 100%
o
Specificity: 98.83%
o
PPV: 96%
o
NPV: 100%
o
Accuracy: 99.09%
Table 6: Cross tabs between FNAC and histopathology result of salivary gland swelling and operated at SPHMMC, Addis Ababa Ethiopia, 2022.
|
Biopsy benign |
||||
|
FNAC benign |
No |
Yes |
Total |
|
|
No |
50 |
2 |
52 |
|
|
Yes |
4 |
54 |
58 |
|
|
Total |
54 |
56 |
110 |
|
|
Biopsy malignant |
||||
|
FNAC malignant |
No |
Yes |
Total |
|
|
No |
78 |
5 |
83 |
|
|
Yes |
2 |
25 |
27 |
|
|
Total |
80 |
30 |
110 |
|
|
Biopsy non neoplastic |
||||
|
FNAC non-neoplastic |
No |
Yes |
Total |
|
|
No |
85 |
0 |
85 |
|
|
Yes |
1 |
24 |
25 |
|
|
Total |
86 |
24 |
110 |
|
Table 7: Parameters of validity measurement for non-neoplastic, benign and malignant FNAC result of salivary gland swelling in comparison with histopathology result, SPHMMC, Addis Ababa, Ethiopia, 2022.
|
Parameters of validity |
Value (%) |
||
|
Non-neoplastic |
Benign |
Malignant |
|
|
Sensitivity |
100% |
96.42% |
83.30% |
|
Specificity |
98.83% |
92.60% |
95.50% |
|
Positive predictive
value |
96% |
93.10% |
92.60% |
|
Negative predictive
value |
100% |
96.10% |
93.97% |
|
Accuracy |
99.09% |
94.51% |
93.63% |
4.
Discussion
Fine
Needle Aspiration Cytology (FNAC) is a widely used diagnostic technique for
evaluating salivary gland enlargement, offering a simple, rapid, and safe
procedure. FNAC is known for its high sensitivity, specificity, and accuracy, with
sensitivity ranging from 86% to 100% and specificity from 90% to 100% in
diagnosing salivary gland lesions1,2,8.
The accuracy of FNAC is significantly influenced by the experience of both the
pathologist and the clinician performing the aspiration1. FNAC plays a crucial role in treatment
planning, helping to avoid unnecessary surgeries and reducing hospital costs9.
In
our study, patients ranged in age from 12 to 79 years, with a mean age of 37.5
years, and a male-to-female ratio of 1:1. Previous studies in Nepal reported a
similar age range, with a median of 38 years7. Research from Liaquat National
Hospital indicated an average age of 42 years (±21),
with a male-to-female ratio of 1:1, while another study reported a mean age of
35.7 years (±19.3 years) and a male-to-female
ratio of 1.2:1. Additionally, research in Tanzania indicated a peak age range
between 20 and 49 years, with a male-to-female ratio of 1.5:17,11-14.
Regarding
the distribution of salivary gland swellings, our study found that 46.4% of
swellings were in the parotid gland, 42.7% in the submandibular gland, 10.9% in
the minor salivary glands, and 0% in the sublingual gland. Other studies have
reported comparable findings, with one study showing 68% parotid gland
involvement, 30% submandibular, 2% minor salivary gland, and 0% sublingual
involvement14,16. Another study
indicated 48.3% parotid, 41.2% submandibular, and 10.4% minor salivary gland
involvement, again with no sublingual gland involvement.
In
terms of the final pathological diagnosis, our study identified 30 malignant
tumors (27.3%), 56 benign tumors (50.9%), and 24 non-neoplastic lesions
(21.8%). A comparable study found that non-neoplastic lesions made up 53.22%
(66/124) of all cases, followed by benign tumors (31.45%, 39/124) and malignant
tumors (15.32%)16. Another study also
found similar proportions, with 27.3% malignant tumors, 50.9% benign tumors,
and 21.8% non-neoplastic lesions15.
The
most frequent pathological findings in our study included pleomorphic adenoma
(benign), mucoepidermoid carcinoma (malignant), and chronic sialadenitis
(non-neoplastic). These findings are consistent with other studies, where
chronic sialadenitis was the most common non-neoplastic lesion, pleomorphic
adenoma was the most common benign lesion, and adenoid cystic carcinoma was the
most frequent malignant lesion7,11,13,17-19.
In one study, non-Hodgkin lymphoma was the most prevalent malignant lesion,
while pleomorphic adenoma was again the most common benign lesion. Another
study found pleomorphic adenoma to be the most common tumor (44.4%), followed
by adenoid cystic carcinoma (24.8%) and mucoepidermoid carcinoma (9.8%).
Pleomorphic adenoma also emerged as the most common neoplasm (63%) in a
separate investigation, with Warthin's tumor accounting for 17.5%.
The
parotid gland was the most frequent site of swelling in our study, consistent
with the findings from Addis Ababa University, where sialadenitis affected
29.8% of patients, with the submandibular gland being the most commonly
affected site20. In our study,
pleomorphic adenoma was the most common lesion in the parotid and minor
salivary glands, while chronic sialadenitis was most frequently found in the
submandibular gland.
Our
diagnostic performance analysis revealed that the sensitivity, specificity, and
accuracy for non-neoplastic lesions were 100%, 98.83%, and 99.09%,
respectively; for benign neoplasms, they were 96.42%, 92.6%, and 94.54%; and
for malignant neoplasms, they were 83.3%, 95.5%, and 94.54% (Tables 5-7). In comparison, other studies have
reported varying values. One study found the sensitivity, specificity, and
accuracy to be 100%, 89.28%, and 91.67% for non-neoplastic lesions; 100%,
86.95%, and 91.67% for benign neoplasms; and 57.14%, 100%, and 83.33% for
malignant neoplasms. Another study reported a 100% sensitivity, 95.8%
specificity, and 93% accuracy for non-neoplastic lesions, with 98.78% accuracy
for benign lesions and 77.77% for malignant lesions7,13,14,16.
The Positive Predictive Values and Negative Predictive Values (PPV and NPV) in our study were 93.1% and 96.1% for benign lesions, 92.6% and 93.97% for malignant lesions, and 96% and 100% for non-neoplastic lesions. One study reported PPV and NPV for benign and malignant tumors as 94.36% and 96.55%, respectively, with 93.33% PPV and 95.29% NPV for malignant tumors. Another study found FNAC to have a 97% negative predictive value (NPV), with a PPV of 92.3% and NPV of 93.6%6,14,18.
5.
Strengths and Limitations
The
main strength of this study is its contribution to understanding the diagnostic
accuracy of FNAC for salivary gland swellings. Given that incisional biopsy is
not recommended for these conditions, FNAC plays a pivotal role in influencing
the surgical approach, providing a reliable foundation for treatment planning.
Our findings underscore the usefulness of FNAC in guiding surgical decisions,
thereby reducing unnecessary procedures and minimizing hospital costs.
However, the study has some limitations:
Lack
of immunohistochemistry: We did not utilize Immunohistochemistry
(IHC), which could have provided further insights into the various histologic
categories and their precise classifications.
Retrospective
data: Since the study was based on retrospectively
collected data, the validity measurements might be either overestimated or
underestimated.
Reliability issues: Due to the retrospective nature of the data, it is difficult to perform reliability testing and to fully assess the causes of false positive and false negative FNAC results.
6. Conclusion
FNAC is a highly sensitive and specific diagnostic tool for salivary gland swellings. It is particularly useful for distinguishing benign from malignant lesions and guiding surgical management.
7. Recommendations
For
healthcare professionals: FNAC should be routinely used for
preoperative evaluation of salivary gland swellings to avoid unnecessary
surgeries.
For
policymakers: Establish pathology laboratories in all
healthcare institutions to improve access to FNAC services.
For researchers: Conduct multicenter studies with larger sample sizes to further validate the diagnostic accuracy of FNAC.
8.
Declarations
Ethical approval was obtained from the Ethical Review Board of Saint Paul’s Hospital Millennium Medical College. Written consent was obtained from patients or their guardians before participation. The confidentiality of patient data was strictly maintained throughout the study. Consent for publication was obtained from the patient and is available upon request from the corresponding author.
9.
Authors' contributions
Dr. Mohammed Sefa Arusi and Dr. Zelalem
Tadesse Wondimu
Ø Substantial
contributions to conception and study design;
Ø drafting
the article and the manuscript
Ø final
approval of the version to be published.
Dr. Zeyneb Saleh
Ø acquisition
of data, or analysis and interpretation of data;
Ø revising
it critically for important intellectual content;
Ø final approval of the version to be published.
10. Acknowledgment: The authors thank St. Paul’s Hospital Millennium Medical College for supporting this study.
11. References
- Singh A, Haritwal A, Murali
BM. Correlation between cytology and histopathology of the salivary gland. Australas Med J. 2011;4: 66-71.
- Koirala S, Sayami G, Pant
AD. Correlation of FNAC and histopathology in diagnosis of salivary gland
lesions. J
Pathology of Nepal. 2014;4: 654-657.
- To VSH, Chan JYW, Tsang RKY,
Wei WI. Review of Salivary Gland Neoplasms. ISRN Otolaryngol. 2012;2012: 1-6.
- Licitra L, Grandi C, Prott FJ, et al. Major and minor
salivary gland tumours. Crit Rev Oncol Hematol. 2003;45: 215-25.
- Sneige N, Batsakis JG, El-Naggar AK. Pathology consultation. Ann Otol Rhinol Laryngol. 1992;101: 877-880.
- Huq AHMZ, Asa A. A
comparative study between fine needle aspiration cytology findings and histopathological
report of major salivary gland neoplasm in a tertiary hospital of Bangladesh. Bangladesh Med Res Counc Bull. 2013;39: 1-6.
- Gupta R, Dewan D, Kumar D,
Suri J. Fine-needle aspiration cytology (FNAC) of salivary gland lesions with
histopathological correlation in a district hospital of Jammu region. Indian J Pathol Oncol. 2016;3(1): 32-36.
- Pantanowitz L, Thompson LDR, Rossi ED. Diagnostic approach to fine needle aspirations of
cystic lesions of the salivary gland. Head Neck Pathol. 2018;12(4): 548-561.
- Das DK, Petkar MA, Al-Mane NM, Sheikh ZA, Mallik MK, Anim JT. Role of fine needle
aspiration cytology in the diagnosis of swellings in the salivary gland
regions: A study of 712 cases. Med
Princ Pract.
2004;13: 95-106.
- Zurrida S, Alasio L, Tradafi
N, Bartoli C, Chiesa F, Pilotti S. Fine-needle aspiration of parotid masses. Ann Surg Oncol. 2010;17: 301-306.
- Masanja MI, Kalyanyama BM, Simon EN. Salivary gland tumors in Tanzania. East Afr Med J. 2003;80: 429-433.
- Aidya S. Correlation of FNAC and histopathology in salivary gland
lesions. J Pathology of Nepal. 2011;1.
- Naz S, Hashmi AA, Khurshid
A, et al. Diagnostic role of fine needle aspiration cytology (FNAC) in the
evaluation of salivary gland swelling: An institutional experience. BMC Res Notes. 2015;8: 1-7.
- Ashraf A, Shaikh AS, Kamal
F, Sarfraz R, Bukhari MH. Diagnostic reliability of FNAC for salivary gland
swellings: A comparative study. Diagn Cytopathol. 2010;38: 499-504.
- Nazir RT, Sharif MA, Iqbal
M, Amin MS. Diagnostic accuracy of fine needle aspiration cytology in hepatic
tumors. J
Coll Physicians Surg Pakistan. 2010;20: 373-376.
- Omhare A, Singh SK, Nigam
JS, Sharma A. Cytohistopathological study of salivary gland lesions in
Bundelkhand Region, Uttar Pradesh, India. Pathol Res Int. 2014;2014: 1-7.
- Liu CC, Jethwa AR, Khariwala
SS, Johnson J, Shin JJ. Sensitivity, specificity, and posttest probability of
parotid fine-needle aspiration: A systematic review and meta-analysis. Otolaryngol Head Neck Surg. 2016;154: 9-23.
- Gudmundsson JK, Ajan A,
Abtahi J. The accuracy of fine-needle aspiration cytology for diagnosis of
parotid gland masses: A clinicopathological study of 114 patients. J Appl Oral Sci. 2016;24: 561-567.
- Poudel A, Shrestha B, Regmi
S. Evaluation of salivary gland lesions by fine needle aspiration cytology at a
tertiary care hospital, Western Nepal. Pathol Lab Med Int. 2020;12: 9-17.
- Beyene M. Prevalence and patterns of salivary gland disease in maxillofacial surgery, affiliated hospital, Addis Ababa, Ethiopia. Addis Ababa University. 2022.
1. Data Collection Format
St. Paul’s
Hospital Millennium Medical College
The Purpose of
this study is to compare and assess sensitivity and specificity of FNAC and
histopathology reports of salivary gland swellings at Saint Paul’s Hospital
Millennium Medical College.
I kindly request
your willingness to perform these reviews. The information gathered will be
used confidentially.
|
Code |
Question |
Response |
Remark
|
|
|
Part one: Socio-demographic factors |
|
|||
|
SD1 |
MRN (code)
|
____________ |
|
|
|
SD2 |
Age
|
____________ |
|
|
|
SD3 |
Sex |
Male |
|
|
|
Female |
|
|||
|
Part two: Clinical characteristics |
|
|||
|
CC1 |
Site of swollen gland
|
Parotid |
|
|
|
submandibular |
|
|||
|
sublingual |
|
|||
|
Minor salivary gland |
|
|
||
|
CC2 |
Side of swelling |
Right |
|
|
|
Left |
|
|||
|
CC3 |
Duration of swelling |
|
||
|
|
||||
|
Part three: Cytopathology pathology (FNAC) findings
|
|
|||
|
CP1 |
FNAC
|
Benign |
|
|
|
Malignant |
|
|||
|
Non neoplastic |
|
|||
|
CP2 |
Benign subtypes |
Pleomorphic adenoma |
|
|
|
Warthin tumor |
|
|||
|
Basal cell adenoma |
|
|||
|
adenoma |
|
|||
|
hemangioma |
|
|||
|
|
|
|||
|
CP3 |
Malignant subtypes
|
Mucoepidermoid carcinoma |
|
|
|
Adenoid cystic carcinoma |
|
|||
|
Squamous cell carcinoma |
|
|||
|
Ex pleomorphic carcinoma |
|
|||
|
adenocarcinoma |
|
|||
|
Basal cell carcinoma |
|
|||
|
Acinar cell carcinoma |
|
|||
|
Ductal carcinoma |
|
|||
|
CP4 |
Non neoplastic
|
mucocele |
|
|
|
Chronic sialadenitis |
|
|||
|
Congenital vascular anomalies |
|
|||
|
Cystic lesion |
|
|||
|
Part four: Histopathology findings |
|
|||
|
HP1 |
Histopathology result |
benign |
|
|
|
malignant |
|
|||
|
Non neoplastic |
|
|||
|
HP2 |
Benign |
Pleomorphic adenoma |
|
|
|
Warthin tumor |
|
|||
|
Basal cell adenoma |
|
|||
|
Adenoma |
|
|||
|
hemangioma
|
|
|||
|
HP3 |
Malignant subtypes |
Mucoepidermoid carcinoma |
|
|
|
Adenoid cystic carcinoma |
|
|||
|
Squamous cell carcinoma |
|
|
||
|
Ex pleomorphic carcinoma |
|
|||
|
adenocarcinoma |
|
|||
|
Basal cell carcinoma |
|
|||
|
Acinar cell carcinoma |
|
|||
|
Ductal carcinoma |
|
|||
|
HP4 |
Non neoplastic |
mucocele |
|
|
|
Chronic sialadenitis |
|
|||
|
Congenital vascular anomalies |
|
|||
|
Cystic lesion |
|
|||