Impacts of Social Determinants of Health (SDoH) on Health Equity
Abstract
Healthcare
access is a universal right for all human beings. The Access to Healthcare in
America report published in 1993 defines access as “the timely use of personal
health services to achieve the best possible health outcomes1.” Access to
health care is important to ensure overall well-being of the population both
physical and mental, detection and treatment of diseases and improve life
expectancy. Even though there is significant investment made in the healthcare
industry to provide quality of care for everyone, access to affordable
healthcare and the subsequent health outcomes are determined by the social and
economic conditions of the members.
Social Determinants of Health, or SDoH, is defined as “Conditions in the places where people live, learn, work, and play which affect a wide range of health and quality-of-life risks and outcomes.” SDoH are non-medical factors that significantly influence health outcomes. Health equity means everyone has a fair and just opportunity to be as healthy as possible. This requires removing obstacles to health care access such as poverty, discrimination, and their consequences, including powerlessness and lack of access to jobs with fair pay, quality education, lack of health insurance and housing, safe environments, and health care. Therefore, there is an urgent need to eliminate health disparities and ensure all people have opportunities to reach their well-being potential.
Keywords: Social Determinants, Health Equity, Economic status, Health outcomes
1.
Introduction
Covid-19
highlighted the unfair treatment, lack of health care accessibility, barriers
to care and structural flaws in the health care system. A study conducted
determined the impacts of SDoH on health outcomes and it concluded that while
clinical care impacts 20 percent on the outcomes, SDoH can impact as much as
50% , further explaining that 47% of the health outcomes is determined by
socio-economic factors compared to individual’s health behavior at 34% ,
clinical care is 16% and finally the physical environment impacts 3% as shown
in the figure 1 below2. Few examples of SDoH that have high impact of quality
of care and health equity include lack of nutritional food resulting in chronic
conditions such as congestive heart disease and diabetes, financial insecurity
due to lack of employment impacting well-being , lack of access to health care
due to affordability ,unsafe housing options and lack of transportation.
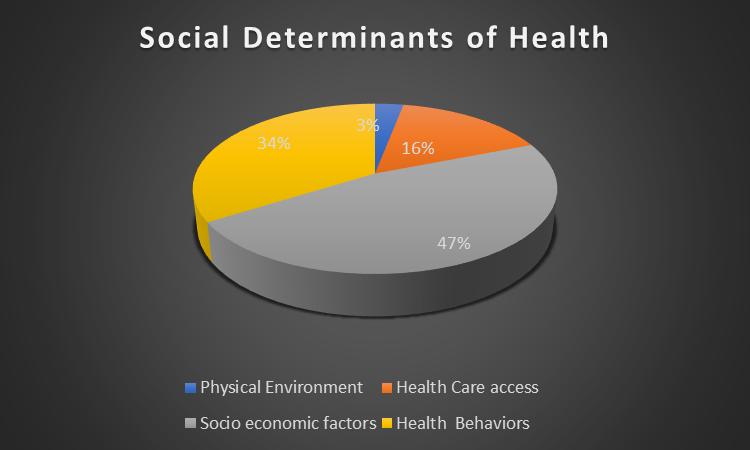
Figure 1: Social determinants of health.
The United States despite spending more money on health care in comparison with other countries in Organization for Economic Co-operation and Development (OECD) has very poor health outcomes and large inequalities when compared to high income countries3.The disparity in health care access has predominant effect on population that face systematic obstacles based on race, religion, economic status ,gender ,geographic location, and other characteristics that are linked to discrimination historically leading to health inequality. The aim of this article is to discuss how SDoH is impacting the access and health care outcomes and the mitigation strategies to improve overall health equity.
2. Impact
of SDoH on Health Equity
The
current health care delivery model in United States is creating a significant
financial burden on the health care eco system and is no longer sustainable.
A model prepared by Deloitte looked at all the high-cost chronic conditions like diabetes, asthma and cancers demonstrate the significant financial burden due to health inequities. The study determined that racial inequity and income disparities are significant factors contributing to late diagnosis resulting in delayed access to appropriate care and medication. The study concluded that for diabetes 4.8% of spending is due to disparities which resulted in $15 billion being spent unnecessarily as against the annual cost of $327 billion . It also noted that black adults are 60% more likely to be diagnosed with diabetes with two or three times with complications due to diabetes than the white adults. The study also revealed that asthma spending due to poverty levels and income disparities is $2.4 US billion as opposed to annual cost of disease. The 4.3% unnecessary spend is due to the income disparities. The figure 2 below sourced from the Deloitte report4 shows how health disparities can increase the health care spending.
Figure 2: How health disparities can increase health care spending
While these numbers do not include costs for mental health, conditions like diabetes and asthma can lead to or worsen depression, anxiety further increasing the cost of care. The issues related to mental health can increase the individual’s susceptibility of developing poor physical health in turn impacting social and cognitive function resulting in unhealthy habits and resort to substance abuse. These types of health inequities would further increase the health care cost in United States projecting a $1 US trillion spend in 2040 compared to $320 US trillion in the present day4.
Though quality health care is an essential right of every individual , research shows that health outcomes are driven by multiple factors, that includes the underlying health behavior, social and environmental factors, and affordable access to health care. To champion “ health equity” ensuring better quality health standards for all individuals, it is important to address the SDoH factors including social , cultural, and environmental that would have tremendous impact on individual’s health outcomes as these factors have around 80% impact on the health outcomes as opposed to the 20% of the individual's overall health. Of 80% of the impacts due to SDoH , environmental factors such as lack to access to food, transportation, housing ,education accounts to 50% and the substance abuse in the form of alcohol and drug consumption accounts for the remaining 30%2.
A study conducted by Hahn and Truman concluded that there is a direct relation between educational attainment and mortality and morbidity. The study showed that people with lower educational attainment has high chances of developing conditions such as diabetes, liver diseases and feeling of worthlessness5. Homelessness is another key factor that has a close influence on poor physical and mental health. There is an increased rate of health issues such as HIV, tuberculosis, substance abuse in homeless people6. Lack of access to nutritional food or food insecurity will have significant impact on health. One study conducted on children revealed that food insecurity was associated with various health issues in children including birth defect, aggression, anxiety, behavioral problems, bad oral health, and high hospitalization7.
Another factor influencing the health outcome is the bias surrounding the individual’s race, ethnicity, language and disability and this bias whether conscious or unconscious creates a segregation among the society. This impacts the way the members are provided with the services resulting in discrimination and lack of fair access to health care resources.
3. Health
Equity Initiatives to Address Disparities in Health Outcomes
Health
equity interventions and programs play a significant role in addressing health
disparities and improving health outcomes by targeting the underlying
determinants and promoting health equity. The main goal of these initiatives is
to create a health care system that is more affordable and ensures everyone has
access to quality care.
3.1.
Community health worker programs
Community
Health Worker programs play a critical role in promoting health equity by
providing community-centered services such as health education , outreach, and
support activities to overcome barriers to health care access in the
underserved communities and address the social determinants that impact health
equity. The CHWs serve as a liaison between the hospitals or the health care
systems and the community-based resources to promote equitable healthcare
delivery. They empower individuals to make healthy choices and raise awareness
about health issues to enable them to take an active role in their well-being.
The CHWs help with a wide range of services from conducting health education
sessions on nutrition, medication adherence, chronic disease management to
helping the members in the health care system navigation in the form scheduling
appointments and monitoring health status for the members with chronic
conditions and provide services in terms of food and transportation. There are
various successful programs such as implemented as part of CHW programs such as
the Bangladesh Rural Advancement Committee (BRAC) Community Health Worker
program was instrumental in reducing the maternal and child mortality rates in
rural Bangladesh through their interventions and programs. During the past
year, the community health workers have provided over 477,000 antenatal care
services, over 255,000 prenatal care services, and delivered 14,000 babies
safely8.
3.2.
Patient navigation programs
Patient
navigation programs play a critical role in promoting health equity by
addressing social, economic, financial, and cultural barriers. It enables
appropriate care and improves health outcomes. These programs measure the
impacts and outcomes using metrics such as utilization, hospital readmissions
and cost savings. The patient navigator or the patient advocates help patients
overcome the barriers, provide them with the diagnosis and treatment options
and necessary access as they navigate the health care ecosystem. The Patient
Navigation programs address a wide range of issues including financial barriers
such as excessive cost of insurance , logistics barriers such as
non-availability of transportation or language issues and social barriers such
as stigma related to seeking mental health services. The results from the
Patient Navigation Research Program (PNRP) set up by National Cancer Institute
showed a decrease in the abnormal cancer screening findings, improved treatment
initiation rates and improved health outcomes among racial and ethnic minority
populations, and patients with economic disparities9.
3.3.
Health education and promotion campaigns
Health
education and promotion campaigns play a significant role in advancing health
equity by promoting health literacy , enabling individuals to make informed
decisions about their health using outreach activities, workshops and targeting
messaging. These foster collaborations with the schools for preventative
screenings, hospitals, and government agencies to enable larger outreach and
create sustainable outreach activities with maximum impact. The campaigns are
tailored considering the unique needs of the communities they are serving
including racial and religious minority groups, low-income communities, LGBTQ,
and individuals with language barriers.
3.4.
Affordable housing, food security and economic development program
Housing
instability and homelessness are the important barriers to quality health care
and affordable housing aims to address this barrier by providing support with
access to subsidized housing units, rental assistance, housing vouchers. The
program also provides supportive services such as mental health management and
case management to individuals experiencing housing instability.
Food security program caters to the dietary and nutritional needs of the members with access to affordable healthy choices in the form of food banks, farmers markets, promoting local food production which is important for maintaining good health. The Supplemental Nutrition Assistance Program (SNAP), the Special Supplemental Nutrition Program for Women, Infants, and Children (WIC), and school meal programs are few food security programs aimed to support with financial assistance for low-income groups.
Economic development initiatives support job opportunities and provide training programs for jobs, small business support programs thus reducing economic disparity by creating a steady source of income to the underserved communities.
3.5.
Policy and advocacy efforts
Policy
and Advocacy efforts are particularly important to address the barriers that
exist in the communities when it comes to health care access and provide
equitable resources and services in the form of regulations and laws at every
level both locally and nationally. Strategic partnerships with decision-makers,
health care organizations, local communities and advocacy groups can help with
grassroot campaigns to raise awareness and build support for initiatives that
would promote health equity. It is important to monitor the impacts of these
initiatives periodically and identify areas for improvement to ensure that
these policies can mitigate the barriers in achieving health equity.
4.
Conclusion
Addressing
socio, economic and environmental related issues is crucial to attain health
equity. This requires a multi prong top-down approach that includes regulatory
and policy changes that would ensure universally accessible healthcare and the
creation of health programs for the underserved communities. Provide
sustainable conditions so the members have access to nutritious diet,
transportation to hospitals, access to care coordinators, and health literacy
so the communities are empowered to make informed health decisions. By
addressing the underlying determinants of health equity, a more equitable
healthcare system that promotes quality of care and health outcomes can be
created.
5.
References
- M.
Millman. “Summary” In: Access to Health Care in America, Washington, DC:
National Academies Press, 1993; 4.
- C Hood, K
Gennuso, G Swain et al. County Health Rankings Relationships Between
Determinant Factors and Health Outcomes. American Journal of Preventive
Medicine, 2015; 50: 2.
- JL Flaubert,
SL Menestrel, D R Williams. Wakefield, Social Determinants of Health and Health
Equity. National Academies Press (US), 2021.
- https://www2.deloitte.com/us/en/insights/industry/health-care/economic-cost-of-health-disparities.html
- RA Hahn, BI
Truman. Education Improves Public Health and Promotes Health Equity.
International Journal of Health Services, 2025; 45, no. 4: 657-678.
- H Sutherland,
MM Ali, E Rosenoff. Individuals experiencing homelessness are likely to have
medical conditions associated with severe illness from
COVID-19. ASPE, 2020.
- C Gundersen,
JP Ziliak. Food Insecurity And Health Outcomes. Health Affairs, 2025; 34: 11.
- https://www.brac.net/program/health/maternal-neonatal-and-child-health/
- H Freeman. The origin, evolution, and principles of patient navigation. Cancer Epidemiology Biomarkers & Prevention, 2012; 21: 1614-1617.
- JL Flaubert,
SL Menestrel, DR Williams et al. Social determinants of health and health
equity. National Academies Press (US), 2021.